Difference between revisions of "Lymphoma"
(→Adult T-cell leukemia/lymphoma: fix ref.) |
|||
| (47 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
[[Image:Lymphoma macro.jpg | thumb | 200px | right | Lymphoma at [[cut-up]]. (WC/Emmanuelm)]] | |||
'''Lymphoma''' is almost a specialty for itself. It can be subclassified a number of ways. | '''Lymphoma''' is almost a specialty for itself. It can be subclassified a number of ways. | ||
| Line 4: | Line 5: | ||
A general introduction to haematopathology is in the ''[[haematopathology]]'' article. | A general introduction to haematopathology is in the ''[[haematopathology]]'' article. | ||
==General== | |||
The presentations are variable and similar to that of other malignancies. They may include: | |||
*Mass effect. | |||
*Weight loss. | |||
*Fever. | |||
*Night sweats. | |||
*Infection. | |||
*Incidental: | |||
**Routine blood work for something unrelated. | |||
**Life insurance work-up. | |||
===B symptoms=== | |||
*May be seen in [[Hodgkin lymphoma]] and non-Hodgkin lymphoma. | |||
*Presence correlates with higher stage. | |||
*Predictor of poor prognosis independent of stage. | |||
All of 'em are required to call "B symptoms"<ref name=pmid5121694>{{Cite journal | last1 = Carbone | first1 = PP. | last2 = Kaplan | first2 = HS. | last3 = Musshoff | first3 = K. | last4 = Smithers | first4 = DW. | last5 = Tubiana | first5 = M. | title = Report of the Committee on Hodgkin's Disease Staging Classification. | journal = Cancer Res | volume = 31 | issue = 11 | pages = 1860-1 | month = Nov | year = 1971 | doi = | PMID = 5121694 | URL = http://cancerres.aacrjournals.org/cgi/pmidlookup?view=long&pmid=5121694 }}</ref> - mnemonic ''These '''B'''othersome features cause '''W'''ednesday '''N'''ight '''F'''ever'':<ref>URL: [http://www.internalizemedicine.com/2011/12/bury-buzzword-b-symptoms.html http://www.internalizemedicine.com/2011/12/bury-buzzword-b-symptoms.html]. Accessed on: 28 March 2012.</ref> | |||
*Weight loss - >10% in 6 months. | |||
*Night sweats. | |||
*Fever - 38 degree C that is unexplained. | |||
Note: | |||
*''A symptoms'' do '''not''' exist. The term comes from the staging system. In the "A" of the staging system the above symptoms are '''a'''bsent. | |||
==Lymphoma classification== | ==Lymphoma classification== | ||
Lymphomas can be divided into: | Lymphomas can be divided into: | ||
*Hodgkin's lymphoma. | *[[Hodgkin's lymphoma]]. | ||
*Non-Hodgkin's lymphoma (NHL). | *Non-Hodgkin's lymphoma (NHL). | ||
| Line 15: | Line 40: | ||
Two most common NHLs: | Two most common NHLs: | ||
*Follicular lymphoma (FL). | *[[Follicular lymphoma]] (FL). | ||
*Diffuse large B-cell lymphoma (DLBCL). | *[[Diffuse large B-cell lymphoma]] (DLBCL). | ||
===Leukemia as a med student=== | ===Leukemia as a med student=== | ||
| Line 22: | Line 47: | ||
*[[Acute myeloid leukemia]] (AML). | *[[Acute myeloid leukemia]] (AML). | ||
*[[Chronic myeloid leukemia]] (CML). | *[[Chronic myeloid leukemia]] (CML). | ||
*Chronic | *[[Chronic lymphocytic leukemia]] (CLL) - relatively good prognosis. | ||
===Histologic classification=== | ===Histologic classification=== | ||
| Line 59: | Line 84: | ||
|} | |} | ||
===Histologic terms=== | ====Histologic terms==== | ||
*Lymphomas = cells look discohesive, may be difficult to differentiate from poor differentiated carcinoma. | *Lymphomas = cells look discohesive, may be difficult to differentiate from poor differentiated carcinoma. | ||
*Auer rods = | *[[Auer rods]] = [[acute myeloid leukemia]]. | ||
**Granular cytoplasmic rod (0.5-1 x4-6 micrometres). | **Granular cytoplasmic rod (0.5-1 x4-6 micrometres). | ||
**Not pathognomonic. | |||
*Reed-Sternberg cells = [[Hodgkin's lymphoma]]. | *Reed-Sternberg cells = [[Hodgkin's lymphoma]]. | ||
**Large cell - very large nucleus. | **Large cell - very large nucleus. | ||
| Line 79: | Line 105: | ||
Others: | Others: | ||
*AE1/AE3 -- to r/o carcinoma. | *[[AE1/AE3]] -ve -- to r/o carcinoma. | ||
====T cell markers==== | ====T cell markers==== | ||
| Line 114: | Line 140: | ||
====Follicular dendritic cells==== | ====Follicular dendritic cells==== | ||
*CD23 -- follicular dendritic cells. | *CD23 -- follicular dendritic cells. | ||
*CD21 -- follicular dendritic cells. | *CD21 -- follicular dendritic cells, considered more sensitive than CD23.<ref name=pmid16280657>{{Cite journal | last1 = Troxell | first1 = ML. | last2 = Schwartz | first2 = EJ. | last3 = van de Rijn | first3 = M. | last4 = Ross | first4 = DT. | last5 = Warnke | first5 = RA. | last6 = Higgins | first6 = JP. | last7 = Natkunam | first7 = Y. | title = Follicular dendritic cell immunohistochemical markers in angioimmunoblastic T-cell lymphoma. | journal = Appl Immunohistochem Mol Morphol | volume = 13 | issue = 4 | pages = 297-303 | month = Dec | year = 2005 | doi = | PMID = 16280657 }}</ref> | ||
====Hodgkin's lymphoma==== | ====Hodgkin's lymphoma==== | ||
| Line 139: | Line 165: | ||
*TdT. | *TdT. | ||
*CD34. | *CD34. | ||
===Molecular pathology=== | |||
{{Main|Molecular pathology}} | |||
{{Main|Molecular pathology tests}} | |||
*T cell clonality study. | |||
*B cell clonality study. | |||
====Chromosomal translocations==== | |||
{{Main|Chromosomal_translocations#Lymphoma}} | |||
==Hodgkin's lymphoma== | ==Hodgkin's lymphoma== | ||
| Line 222: | Line 257: | ||
==Intravascular lymphoma== | ==Intravascular lymphoma== | ||
*[[AKA]] ''angiotropic lymphoma'', ''intravascular malignant lymphomatosis'', ''malignant angioendotheliomatosis'' | |||
*Rare. | *Rare. | ||
*Usually B-cell lineage (see | *Usually B-cell lineage (see ''[[intravascular large B-cell lymphoma]]''). | ||
**May be T-cell lineage.<ref name=pmid20337769>{{cite journal |author=Wang L, Li C, Gao T |title=Cutaneous intravascular anaplastic large cell lymphoma |journal=J Cutan Pathol |volume= |issue= |pages= |year=2010 |month=March |pmid=20337769 |doi=10.1111/j.1600-0560.2010.01538.x |url=}}</ref> | **May be T-cell lineage.<ref name=pmid20337769>{{cite journal |author=Wang L, Li C, Gao T |title=Cutaneous intravascular anaplastic large cell lymphoma |journal=J Cutan Pathol |volume= |issue= |pages= |year=2010 |month=March |pmid=20337769 |doi=10.1111/j.1600-0560.2010.01538.x |url=}}</ref> | ||
==Burkitt's lymphoma== | ==Burkitt's lymphoma== | ||
| Line 312: | Line 312: | ||
**Images: [http://en.wikipedia.org/wiki/File:Auer_rods.PNG Auer rods (WP)], [http://www.healthsystem.virginia.edu/internet/hematology/HessImages/Acute-myelogenous-leukemia-M4-100x-Auer-rods-website-arrow.jpg Auer rods (virginia.edu)]. | **Images: [http://en.wikipedia.org/wiki/File:Auer_rods.PNG Auer rods (WP)], [http://www.healthsystem.virginia.edu/internet/hematology/HessImages/Acute-myelogenous-leukemia-M4-100x-Auer-rods-website-arrow.jpg Auer rods (virginia.edu)]. | ||
==Enteropathy-associated T cell lymphoma | ==Enteropathy-associated T-cell lymphoma== | ||
*Abbreviated ''EATL''. | *Abbreviated ''EATL''. | ||
*[[AKA]] ''enteropathy-type T cell lymphoma'' (ETTL). | *[[AKA]] ''enteropathy-type T-cell lymphoma'' (ETTL). | ||
{{Main|Enteropathy-associated T-cell lymphoma}} | |||
==Angioimmunoblastic T-cell lymphoma== | ==Angioimmunoblastic T-cell lymphoma== | ||
| Line 335: | Line 327: | ||
Features: | Features: | ||
*Intermediate size cells with: | *Intermediate size cells with: | ||
**+/-Vesicular nuclei. | **+/-[[Vesicular nuclei]]. | ||
**Clear, moderate cytoplasm. | **Clear, moderate cytoplasm. | ||
*"Empty" sinus; subcapsular sinuses "open". | *"Empty" sinus; subcapsular sinuses "open". | ||
| Line 364: | Line 356: | ||
*Abbreviated ''PMBL''. | *Abbreviated ''PMBL''. | ||
*[[AKA]] ''primary mediastinal large B-cell lymphoma''. | *[[AKA]] ''primary mediastinal large B-cell lymphoma''. | ||
{{Main|Primary mediastinal B-cell lymphoma}} | |||
==Anaplastic large cell lymphoma== | ==Anaplastic large cell lymphoma== | ||
*Abbreviated ''ALCL''. | *Abbreviated ''ALCL''. | ||
{{Main|Anaplastic large cell lymphoma}} | |||
==Cutaneous T cell lymphoma== | ==Cutaneous T cell lymphoma== | ||
| Line 457: | Line 391: | ||
===IHC=== | ===IHC=== | ||
* | *CD57 +ve -- '''important'''. | ||
*CD3 +ve. | |||
*CD5 +ve. | |||
*CD45 +ve. | |||
==Lymphoplasmacytic lymphoma== | ==Lymphoplasmacytic lymphoma== | ||
:''Waldenström macroglobulinemia'' redirects here. | |||
===General=== | ===General=== | ||
Features:<ref name=Ref_PCPBoD8_325>{{Ref PCPBoD8|325}}</ref> | Features:<ref name=Ref_PCPBoD8_325>{{Ref PCPBoD8|325}}</ref> | ||
| Line 466: | Line 403: | ||
*Secretes monoclonal IgM. | *Secretes monoclonal IgM. | ||
Clinical:<ref name=Ref_PCPBoD8_325>{{Ref PCPBoD8|325}}</ref> | Note: | ||
*Symptoms of blood hyperviscosity | *''Waldenström macroglobulinemia'' is a type of lymphoplasmacytic lymphoma<ref name=pmid22507796>{{Cite journal | last1 = Gertz | first1 = MA. | title = Waldenström macroglobulinemia. | journal = Hematology | volume = 17 Suppl 1 | issue = | pages = 112-6 | month = Apr | year = 2012 | doi = 10.1179/102453312X13336169156212 | PMID = 22507796 }}</ref> - it is characterized by: | ||
**''Hyperviscosity syndrome''. | |||
**Bony destruction (seen in [[multiple myeloma]]) is absent.<ref name=Ref_PCPBoD8_325>{{Ref PCPBoD8|325}}</ref> | |||
====Clinical==== | |||
Features:<ref name=Ref_PCPBoD8_325>{{Ref PCPBoD8|325}}</ref> | |||
*Symptoms of blood hyperviscosity - these include: | |||
**Visual impairment. | |||
**Neurologic impairment. | |||
**Bleeding. | |||
**[[Cryoglobulinemia]] - may have ''Raynaud phenomenon''. | |||
*Hemolysis. | *Hemolysis. | ||
*Bence-Jones proteinuria - seen in over half of patients.<ref name=pmid11797112>{{Cite journal | last1 = Kyrtsonis | first1 = MC. | last2 = Vassilakopoulos | first2 = TP. | last3 = Angelopoulou | first3 = MK. | last4 = Siakantaris | first4 = P. | last5 = Kontopidou | first5 = FN. | last6 = Dimopoulou | first6 = MN. | last7 = Boussiotis | first7 = V. | last8 = Gribabis | first8 = A. | last9 = Konstantopoulos | first9 = K. | title = Waldenström's macroglobulinemia: clinical course and prognostic factors in 60 patients. Experience from a single hematology unit. | journal = Ann Hematol | volume = 80 | issue = 12 | pages = 722-7 | month = Dec | year = 2001 | doi = 10.1007/s00277-001-0385-8 | PMID = 11797112 }}</ref> | |||
Treatment: | |||
*Watchful waiting or chemotherapy. | |||
*Hyperviscosity syndrome: plasmapheresis. | |||
===Microscopic=== | ===Microscopic=== | ||
| Line 474: | Line 426: | ||
*Plasmacytoid lymphocytes. | *Plasmacytoid lymphocytes. | ||
*Mixed inflammatory infiltrate with [[mast cell]]s, [[plasma cell]]s, lymphocytes. | *Mixed inflammatory infiltrate with [[mast cell]]s, [[plasma cell]]s, lymphocytes. | ||
DDx: | |||
*[[Plasma cell neoplasm]]. | |||
===IHC=== | ===IHC=== | ||
| Line 499: | Line 454: | ||
*Cloverleaf nuclei. | *Cloverleaf nuclei. | ||
**Nuclei with multiple lobulations. | **Nuclei with multiple lobulations. | ||
Image: | |||
*[http://www.pathpedia.com/education/eatlas/histopathology/blood_cells/adult_t-cell_leukemia_htlv1-positive_acute_form/adult-t-cell-leukemia-htlv1-%5B2-bl095-2%5D.jpeg?Width=600&Height=450&Format=4 Cloverleaf nucleus (pathpedia.com)].<ref>URL: [http://www.pathpedia.com/education/eatlas/histopathology/blood_cells/adult_t-cell_leukemia_htlv1-positive_acute_form.aspx http://www.pathpedia.com/education/eatlas/histopathology/blood_cells/adult_t-cell_leukemia_htlv1-positive_acute_form.aspx]. Accessed on: 7 February 2012.</ref> | |||
===IHC=== | ===IHC=== | ||
| Line 504: | Line 462: | ||
*CD3 +ve. | *CD3 +ve. | ||
*CD5 +ve. | *CD5 +ve. | ||
*CD25 +ve. | *CD25 +ve. | ||
*CD45 +ve. | *CD45 +ve. | ||
*HTLV-1 +ve. | |||
Others:<ref name=pmid19165640/> | Others:<ref name=pmid19165640/> | ||
| Line 520: | Line 478: | ||
*[[AKA]] ''extranodal natural kill lymphoma'' | *[[AKA]] ''extranodal natural kill lymphoma'' | ||
*[[AKA]] ''angiocentric lymphoma''. | *[[AKA]] ''angiocentric lymphoma''. | ||
{{Main|Extranodal NK/T-cell lymphoma, nasal type}} | |||
==Table of lymphoma== | ==Table of lymphoma== | ||
| Line 625: | Line 557: | ||
| lymph node usually, germinal center | | lymph node usually, germinal center | ||
| sheets of large discohesive cells; if only nodular = follicular lymphoma | | sheets of large discohesive cells; if only nodular = follicular lymphoma | ||
| | | MIB1 >40% | ||
| none / like follicular lymphoma t(14,18) / c-MYC (like Burkitt lymphoma) | | none / like follicular lymphoma t(14,18) / c-MYC (like Burkitt lymphoma) | ||
| poor prognosis | | poor prognosis | ||
Latest revision as of 19:37, 31 July 2016
Lymphoma is almost a specialty for itself. It can be subclassified a number of ways.
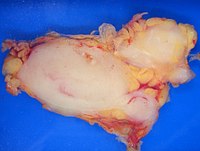
This article is an introduction to lymphoma. An introduction to lymph nodes and lymph node pathology that is not lymphoma are in the articles lymph node and lymph node pathology.
A general introduction to haematopathology is in the haematopathology article.
General
The presentations are variable and similar to that of other malignancies. They may include:
- Mass effect.
- Weight loss.
- Fever.
- Night sweats.
- Infection.
- Incidental:
- Routine blood work for something unrelated.
- Life insurance work-up.
B symptoms
- May be seen in Hodgkin lymphoma and non-Hodgkin lymphoma.
- Presence correlates with higher stage.
- Predictor of poor prognosis independent of stage.
All of 'em are required to call "B symptoms"[1] - mnemonic These Bothersome features cause Wednesday Night Fever:[2]
- Weight loss - >10% in 6 months.
- Night sweats.
- Fever - 38 degree C that is unexplained.
Note:
- A symptoms do not exist. The term comes from the staging system. In the "A" of the staging system the above symptoms are absent.
Lymphoma classification
Lymphomas can be divided into:
- Hodgkin's lymphoma.
- Non-Hodgkin's lymphoma (NHL).
Other categorizations:
- T cell lymphomas (rare).
- B cell lymphomas (more common).
Two most common NHLs:
- Follicular lymphoma (FL).
- Diffuse large B-cell lymphoma (DLBCL).
Leukemia as a med student
- Acute lymphoid leukemia (ALL) - predominantly in smALL people, i.e. children.
- Acute myeloid leukemia (AML).
- Chronic myeloid leukemia (CML).
- Chronic lymphocytic leukemia (CLL) - relatively good prognosis.
Histologic classification
- "Size".
- Nodularity.
"Size"
- The single most important factor for classifying lymphomas.
- Not really based on size.
| "Large" | "Small" | Utility | |
| Nucleoli | present | absent | most discriminative |
| Size | >2x RBC dia. | <2x RBC dia. | moderate |
| Chromatin pattern | "open" (pale) | "closed" | moderate/minimal |
| Cytoplasm | mold-minimal basophilic cytoplasm |
scant cytoplasm | minimal |
Histologic terms
- Lymphomas = cells look discohesive, may be difficult to differentiate from poor differentiated carcinoma.
- Auer rods = acute myeloid leukemia.
- Granular cytoplasmic rod (0.5-1 x4-6 micrometres).
- Not pathognomonic.
- Reed-Sternberg cells = Hodgkin's lymphoma.
- Large cell - very large nucleus.
- Classically binucleated.
- Large cell - very large nucleus.
- Russell bodies = plasmacytoma (+others).
- Effacement of nodal architecture.
- Loss of proliferation centers.
IHC
General
- CD45.
- AKA common lymphocyte antigen.
- Useful to differentiate from carcinomas (e.g. small cell carcinoma).
Others:
- AE1/AE3 -ve -- to r/o carcinoma.
T cell markers
- CD2 -- T cell marker (all T cells).
- CD3 -- T cell marker (all T cells).
- CD4 -- subset of T cells.
- CD8 -- subset of T cells.
- CD7 -- often lost first in T cell lymphomas.
- CD5 -- +ve in CLL & mantle cell lymphoma.
- CD43 -- +ve in mantle cell lymphoma
- ALK1[4] - prognostic in anaplastic large cell lymphoma (ALCL).[5]
- TIA1 - cytotoxic T-cell.[6]
- Granzyme B.
B cell markers
- CD20 -- B cell marker.
- CD19 -- B cell marker - used for flow cytometry.
- PAX5 -- nuclear staining.[7]
- Image: PAX5 in Hodgkin's lymphoma.
- CD79a.
- CD10 -- follicle center.
- BCL6 -- follicle center.
- BCL2 -- normally negative in germinal centers (GCs), marks T cell; +ve in small B cell lymphomas.
- MUM1 -- -ve in follicular lymphoma, +ve in DLBCL that did not arise from follicular lymphoma.
Plasma cell
- Kappa -- usu. slightly stronger than lambda.
- Lambda.
- CD56[8] -- also +ve in NK/T cell lymphomas.
- CD57 -- +ve in T-cell large granular lymphocytic leukemia.[9].
- CD138.
Follicular dendritic cells
- CD23 -- follicular dendritic cells.
- CD21 -- follicular dendritic cells, considered more sensitive than CD23.[10]
Hodgkin's lymphoma
Classic
- CD30 +ve -- Hodgkin's lymphoma (most sensitive).
- CD15 +ve.
- PAX5 +ve.
- EMA -ve.
- EBER +ve/-ve.
Others:
- CD20, CD45: weak +ve or -ve.
NLPHL
- CD20 +ve.
- CD30 -ve, CD15 -ve.
- EMA +ve/-ve.
- EBER -ve.
Others
- Myeloperoxidase - in PMNs.
- Glycophorin C.
- CD61 -- megakaryocytes.
- TdT.
- CD34.
Molecular pathology
- T cell clonality study.
- B cell clonality study.
Chromosomal translocations
Hodgkin's lymphoma
General
- Abbreviated HL.
Microscopic
By definition, HL has Reed-Sternberg cells (RSCs).
Classical HL
Features (classic HL):
- Reed-Sternberg cell.
- Large binucleated cell.
- May be multinucleated.
- May have a horseshoe-like shape.
- Macronucleolus - approximately the size of a RBC (~8 micrometers).
- Well-defined cell border.
- Large binucleated cell.
Notes:
- Large mononuclear cells are common (so called "mononuclear RSCs") but not diagnostic.
Images (classic HL):
- HL mixed cellularity - cytology (WC).
- HL mixed cellularity - cytology (WC).
- HL mixed cellularity (WC).
Subtypes
There are four CHL subtypes:[11]
- Nodular sclerosis CHL - ~70% of CHL.
- Mixed cellular background - T cell, plasma cells, eosinophils, neutrophils and histiocytes.
- Nodular sclerosing fibrosis - thick strands fibrosis.
- Mixed cellularity CHL - ~20-25% of CHL.
- Like nodular sclerosis - but no fibrosis.
- May be associated with HIV infection.[12]
- Lymphocyte-rich CHL - rare.
- T lymphocytes only (no mix of cells).
- Lymphocyte-depleted CHL - rare.
Memory device:
- The subtypes prevalence is in reverse alphabetical order.
Nodular lymphocyte-predominant HL
Features (nodular lymphocyte-predominant Hodgkin's lymphoma):
- Popcorn cell (previously known as Lymphocytic & histiocytic cell (L&H cell)[13]) - variant of RSC:
- Cells (relatively) small (compared to classic RSCs).
- Lobulated nucleus - key feature.
- Small nucleoli.
- Subtle nodularity at low power (2.5x or 5x objective).
Images (NLPHL):
Small cell lymphomas
This grouping includes:
- Follicular lymphoma.
- Marginal zone lymphoma.
- Nodal marginal zone lymphoma.
- Extranodal marginal zone lymphoma (MALT lymphoma).
- Splenic marginal zone lymphoma.
- Mantle zone lymphoma.
- Small lymphocytic lymphoma (SLL) / chronic lymphocytic leukemia (CLL).
- Hairy cell leukemia.
Diffuse large B-cell lymphoma
General
- Abbreviated DLBCL.
Microscopic
Features:[14]
- Large cells -- 4-5 times the diameter of a small lymphocytes.
- Typically have marked cell-to-cell variation in size and shape.
- Cytoplasm usu. basophilic and moderate in abundance.
- +/-Prominent nucleoli, may be peripheral and/or multiple.
Notes:
- Large bizarre cells can occasionally mimic Reed-Sternberg cells, seen in Hodgkin lymphoma.
Intravascular lymphoma
- AKA angiotropic lymphoma, intravascular malignant lymphomatosis, malignant angioendotheliomatosis
- Rare.
- Usually B-cell lineage (see intravascular large B-cell lymphoma).
- May be T-cell lineage.[15]
Burkitt's lymphoma
General
- Abbreviated BL.
- Subtyped by etiology.
Microscopic
Features:
- "Starry-sky pattern":
- The stars in the pattern are: tingible-body macrophages.
- Tingible-body macrophages = macrophages containing apoptotic tumour cells.
- The tumour cells are the sky.
- The stars in the pattern are: tingible-body macrophages.
- Tumour cells:[16]
- Medium-sized (~1.5-2x the size of a RBC) with uniform size ("monotonous") -- key feature.
- Round nucleus.
- Small nucleoli.
- Relatively abundant cytoplasm.
- Brisk mitotic rate.
Plasma cell neoplasms
- These arise from plasma cells.
- AKA plasma cell myeloma, plasmacytoma.
- Multiple myeloma (a clinical diagnosis) fits into this category.
Acute myeloid leukemia
General
- May afflicits young adult.
- Males>females.
Complications
- Chloroma - soft tissue mass.
- Leukostasis.
- Occurs - lungs and brain.[17]
- Hyperviscosity syndrome.
- Spontaneous bleeding with low platelet counts.
Classification
There are two classifications:
- FAB (French-American-British) - based on histologic appearance/maturation.
- WHO classification.
Histology
- Auer rods - not required to diagnose.[18]
- Cytoplasmic granular rods in blast cells.
- Dimensions: approx. 0.5-1 x 4-6 micrometres.
- Images: Auer rods (WP), Auer rods (virginia.edu).
- Cytoplasmic granular rods in blast cells.
Enteropathy-associated T-cell lymphoma
- Abbreviated EATL.
- AKA enteropathy-type T-cell lymphoma (ETTL).
Angioimmunoblastic T-cell lymphoma
- Abbreviated AITL.
General
- Rare.
- Common among T-cell lymphomas.
- Middle age or elderly.
Microscopic
Features:
- Intermediate size cells with:
- +/-Vesicular nuclei.
- Clear, moderate cytoplasm.
- "Empty" sinus; subcapsular sinuses "open".
Images:
IHC
Features - positives:[19]
- CD3 +ve.
- CD5 +ve.
- CD43 +ve.
Others:
- CD4 +ve and CD8 +ve with CD4>CD8.
- CD20 +ve/-ve!
- CD10 +ve/-ve!
- CD21 +ve -- prominent FDC meshworks;[20] tumour cell not +ve.
Negatives:
Primary mediastinal B-cell lymphoma
- Abbreviated PMBL.
- AKA primary mediastinal large B-cell lymphoma.
Anaplastic large cell lymphoma
- Abbreviated ALCL.
Cutaneous T cell lymphoma
General
- Abbreviated as CTCL.
- Sézary syndrome is a subset of CTCL.
Microscopic
Features:[21]
Images:
T-cell large granular lymphocytic leukemia
General
- May be seen in the context of Felty syndrome.
Microscopic
Features:
- Large cell lymphoma.
Images:
IHC
- CD57 +ve -- important.
- CD3 +ve.
- CD5 +ve.
- CD45 +ve.
Lymphoplasmacytic lymphoma
- Waldenström macroglobulinemia redirects here.
General
Features:[24]
- B cell neoplasm.
- Secretes monoclonal IgM.
Note:
- Waldenström macroglobulinemia is a type of lymphoplasmacytic lymphoma[25] - it is characterized by:
- Hyperviscosity syndrome.
- Bony destruction (seen in multiple myeloma) is absent.[24]
Clinical
Features:[24]
- Symptoms of blood hyperviscosity - these include:
- Visual impairment.
- Neurologic impairment.
- Bleeding.
- Cryoglobulinemia - may have Raynaud phenomenon.
- Hemolysis.
- Bence-Jones proteinuria - seen in over half of patients.[26]
Treatment:
- Watchful waiting or chemotherapy.
- Hyperviscosity syndrome: plasmapheresis.
Microscopic
Features:[24]
- Plasmacytoid lymphocytes.
- Mixed inflammatory infiltrate with mast cells, plasma cells, lymphocytes.
DDx:
IHC
Features:[27]
- PAX5 +ve.
- CD20 +ve.
- CD38 +ve.
- CD138 +ve.
Others:[27]
- CD5 -ve.
- CD10 -ve.
- CD23 -ve.
- CyclinD1 -ve.
- CD3 -ve.
- CD7 -ve.
Adult T-cell leukemia/lymphoma
General
- Etiology: Human T-cell Lymphoma Virus 1 (HTLV-1).[28]
- Poor prognosis ~ 1 year survival with treatment.
Microscopic
Features:[29]
- Cloverleaf nuclei.
- Nuclei with multiple lobulations.
Image:
IHC
Features:[31]
- CD3 +ve.
- CD5 +ve.
- CD25 +ve.
- CD45 +ve.
- HTLV-1 +ve.
Others:[31]
- CD7 -ve.
- CD20 -ve.
- CD79a -ve.
Hepatosplenic T-cell lymphoma
Extranodal NK/T-cell lymphoma, nasal type
Table of lymphoma
B cell lymphomas
| Name | Size of cells | Site | Histomorphology | IHC | Translocations | Clinical | Prevalence | DDx |
|---|---|---|---|---|---|---|---|---|
| Follicular lymphoma | small (centrocytes) | lymph node, germinal center | abundant atypical follicles (lack GC polarity, lack polar mantle zone), effaced sinuses, scattered large cells (centroblasts) | CD10+, bcl-6+[32] | t(14,18) | usually indolent, may transform to DLBCL | very common | DLBCL, other small cell lymphomas |
| Mantle cell lymphoma | small, monomorphic | lymph node, mantle zone | monomorphic lymphoid, abundant mitoses. +/-scattered epithelioid histiocytes, sclerosed blood vessels | CD5+, CD23-, CD43+, cyclin D1+[32] | t(11;14)(q13;q32)[33] | indolent ??? | uncommon | other small cell lymphomas, PTGC, Castleman disease, Burkitt's lymphoma |
| Extranodal marginal zone lymphoma (MALT lymphoma) | small | mucosa-associated lymphoid tissue, GI tract + elsewhere | +/- lymphepithelial lesion (cluster of 3+ cells in epithelium) | CD21+, CD11c+, CD5-, CD23-[32] | ??? | indolent ??? | common | other small cell lymphomas, neuroendocrine tumours |
| Precursor B-cell lymphoblastic lymphoma/ leukemia | small | lymph node ???, bone marrow | nuclei slightly large than resting lymphocytes, scant basophilic cytoplasm, irregular nuclear membrane, no nucleoli, stippled chromatin[34] | CD10+, CD5-, TdT+, CD99+[32] | +/-t(12;21)[35] | aggressive ??? | uncommon | small cell lymphomas |
| Hairy cell leukemia | small | bone marrow, peripheral blood | perinuclear clearing, clear cytoplasm, central nucleus | CD25+, CD103+, CD5-[36] | translocations ? | splenomegaly, no lymphadenopathy, pancytopenia, good prognosis with Tx | uncommon | small cell leukemias/lymphomas (e.g. SMZL) |
| Burkitt's lymphoma | medium, monomorphic | lymph node, germinal center (???) | tingible-body macrophages ("starry sky" appearance), round nucleus, small nucleoli, mitoses +++ | CD10+, BCL6+, BCL2- | t(8;14) (q24;q32) | rapid growth, may be associated with EBV, HIV/AIDS | uncommon | DLBCL, mantle cell lymphoma |
| Diffuse large B cell lymphoma | large cells (>2x RBC, often larger), variable size | lymph node usually, germinal center | sheets of large discohesive cells; if only nodular = follicular lymphoma | MIB1 >40% | none / like follicular lymphoma t(14,18) / c-MYC (like Burkitt lymphoma) | poor prognosis | very common | Burkitt lymphoma, ALCL, Hodgkin lymphoma |
| Primary mediastinal B-cell lymphoma | large (>2x RBC, often larger), variable size | mediastinum | histomorphology ? | IHC ? | translocations ? | predominantly young adults, better prognosis than DLBCL | uncommon | DLBCL |
| B cell small lymphocytic lymphoma / chronic lymphocytic leukemia |
small | lymph node (???) | proliferation centres | CD5+, CD23+, CD43+, cyclin D1- | trisomy 12; deletions of 11q, 13q, 17p[37] | good prognosis / indolent course | common | other small cell lymphomas |
T cell lymphomas
| Name | Size of cells | Site | Histomorphology | IHC | Translocations | Clinical | Prevalence | DDx |
|---|---|---|---|---|---|---|---|---|
| Angioimmunoblastic lymphoma | size of cells ? | site ? | histomorphology ? | IHC ? | translocations ? | clinical ? | prevalence ? | DDx ? |
| Enteropathy-type T cell lymphoma | size of cells ? | site ? | histomorphology ? | IHC ? | translocations ? | clinical ? | prevalence ? | DDx ? |
| Precursor lymphoblastic lymphoma / leukemia | size of cells ? | site ? | histomorphology ? | IHC ? | translocations ? | clinical ? | prevalence ? | DDx ? |
| Adult T-cell lymphoma / leukemia | size of cells ? | site ? | cloverleaf nuclei (multilobular nuclei) | IHC ? | translocations ? | poor prognosis ~ 1 year survival w/ Tx; d/t HTLV-1 | prevalence ? | DDx ? |
| Peripheral T cell lymphoma (NOS) | size of cells ? | site ? | histomorphology ? | TIA-1+ | translocations ? | clinical ? | prevalence ? | DDx ? |
| Anaplastic large cell lymphoma | large | deep & subcapsular sinuses of LN | eosinophilic cytoplasm, nucleoli, often cohesive, wreath cell (C-shaped nucleus) | CD30+/-, Alk+/-, CD4+, CD3- | t(2,5)(p23;q35)[38] | clinical ? | uncommon | carcinoma |
| Extranodal NK/T cell lymphoma nasal type | large ??? | nasal ??? | histomorphology ? | EBER+, CD16+, CD56+, CD57-, TIA-1+, Granzyme B+ | translocations ? | common in East Asia | uncommon | DDx ? |
| Blastic NK cell lymphoma | size of cells ? | site ? | histomorphology ? | IHC ? | translocations ? | clinical ? | prevalence ? | DDx ? |
See also
- Haematopathology - introduction.
References
- ↑ Carbone, PP.; Kaplan, HS.; Musshoff, K.; Smithers, DW.; Tubiana, M. (Nov 1971). "Report of the Committee on Hodgkin's Disease Staging Classification.". Cancer Res 31 (11): 1860-1. PMID 5121694.
- ↑ URL: http://www.internalizemedicine.com/2011/12/bury-buzzword-b-symptoms.html. Accessed on: 28 March 2012.
- ↑ 3.0 3.1 Alanen A, Pira U, Lassila O, Roth J, Franklin RM (March 1985). "Mott cells are plasma cells defective in immunoglobulin secretion". Eur. J. Immunol. 15 (3): 235–42. PMID 3979421.
- ↑ URL: http://www.ncbi.nlm.nih.gov/omim/601284. Accessed on: 31 August 2010.
- ↑ Pittaluga S, Wlodarska I, Pulford K, et al. (August 1997). "The monoclonal antibody ALK1 identifies a distinct morphological subtype of anaplastic large cell lymphoma associated with 2p23/ALK rearrangements". Am. J. Pathol. 151 (2): 343–51. PMC 1858018. PMID 9250148. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1858018/.
- ↑ URL: http://www.ncbi.nlm.nih.gov/omim/603518. Accessed on: 18 August 2010.
- ↑ URL: http://www.ncbi.nlm.nih.gov/omim/167414. Accessed on: 18 August 2010.
- ↑ URL: http://www.ncbi.nlm.nih.gov/omim/116930. Accessed on: 31 August 2010.
- ↑ URL: http://www.nature.com/bmt/journal/v33/n1/full/1704298a.html. Accessed on: 31 August 2010.
- ↑ Troxell, ML.; Schwartz, EJ.; van de Rijn, M.; Ross, DT.; Warnke, RA.; Higgins, JP.; Natkunam, Y. (Dec 2005). "Follicular dendritic cell immunohistochemical markers in angioimmunoblastic T-cell lymphoma.". Appl Immunohistochem Mol Morphol 13 (4): 297-303. PMID 16280657.
- ↑ Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 567. ISBN 978-0781765275.
- ↑ 12.0 12.1 Sissolak G, Sissolak D, Jacobs P (April 2010). "Human immunodeficiency and Hodgkin lymphoma". Transfus. Apher. Sci. 42 (2): 131–9. doi:10.1016/j.transci.2010.01.008. PMID 20138008.
- ↑ Küppers R, Rajewsky K, Braeuninger A, Hansmann ML (March 1998). "L&H cells in lymphocyte-predominant Hodgkin's disease". N. Engl. J. Med. 338 (11): 763–4; author reply 764–5. doi:10.1056/NEJM199803123381113. PMID 9499174.
- ↑ Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Nelso Fausto; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease (7th ed.). St. Louis, Mo: Elsevier Saunders. pp. 676 (???). ISBN 0-7216-0187-1.
- ↑ Wang L, Li C, Gao T (March 2010). "Cutaneous intravascular anaplastic large cell lymphoma". J Cutan Pathol. doi:10.1111/j.1600-0560.2010.01538.x. PMID 20337769.
- ↑ Bellan C, Lazzi S, De Falco G, Nyongo A, Giordano A, Leoncini L (March 2003). "Burkitt's lymphoma: new insights into molecular pathogenesis". J. Clin. Pathol. 56 (3): 188–92. PMC 1769902. PMID 12610094. http://jcp.bmj.com/cgi/pmidlookup?view=long&pmid=12610094.
- ↑ AML. Harrison's 16th Ed.
- ↑ AG. 8 July, 2009.
- ↑ 19.0 19.1 19.2 19.3 Bal, M.; Gujral, S.; Gandhi, J.; Shet, T.; Epari, S.; Subramanian, PG.. "Angioimmunoblastic T-Cell lymphoma: a critical analysis of clinical, morphologic and immunophenotypic features.". Indian J Pathol Microbiol 53 (4): 640-5. doi:10.4103/0377-4929.72010. PMID 21045384.
- ↑ URL: http://path.upmc.edu/cases/case650/dx.html. Accessed on: 27 January 2012.
- ↑ URL: http://emedicine.medscape.com/article/209091-overview. Accessed on: 19 August 2010.
- ↑ URL: http://emedicine.medscape.com/article/204529-diagnosis. Accessed on: 19 August 2010.
- ↑ URL: http://dictionary.reference.com/browse/convoluted. Accessed on: 19 August 2010.
- ↑ 24.0 24.1 24.2 24.3 Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 325. ISBN 978-1416054542.
- ↑ Gertz, MA. (Apr 2012). "Waldenström macroglobulinemia.". Hematology 17 Suppl 1: 112-6. doi:10.1179/102453312X13336169156212. PMID 22507796.
- ↑ Kyrtsonis, MC.; Vassilakopoulos, TP.; Angelopoulou, MK.; Siakantaris, P.; Kontopidou, FN.; Dimopoulou, MN.; Boussiotis, V.; Gribabis, A. et al. (Dec 2001). "Waldenström's macroglobulinemia: clinical course and prognostic factors in 60 patients. Experience from a single hematology unit.". Ann Hematol 80 (12): 722-7. doi:10.1007/s00277-001-0385-8. PMID 11797112.
- ↑ 27.0 27.1 Liu, EB.; Zhang, PH.; Li, ZQ.; Sun, Q.; Yang, QY.; Fang, LH.; Sun, FJ.; Qiu, LG. (May 2010). "[Clinicopathologic features of lymphoplasmacytic lymphoma].". Zhonghua Bing Li Xue Za Zhi 39 (5): 308-12. PMID 20654153.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 327. ISBN 978-1416054542.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 328. ISBN 978-1416054542.
- ↑ URL: http://www.pathpedia.com/education/eatlas/histopathology/blood_cells/adult_t-cell_leukemia_htlv1-positive_acute_form.aspx. Accessed on: 7 February 2012.
- ↑ 31.0 31.1 Bittencourt, AL.; Barbosa, HS.; Vieira, MD.; Farré, L. (2009). "Adult T-cell leukemia/lymphoma (ATL) presenting in the skin: clinical, histological and immunohistochemical features of 52 cases.". Acta Oncol 48 (4): 598-604. doi:10.1080/02841860802657235. PMID 19165640.
- ↑ 32.0 32.1 32.2 32.3 Lester, Susan Carole (2005). Manual of Surgical Pathology (2nd ed.). Saunders. pp. 95. ISBN 978-0443066450.
- ↑ URL: http://atlasgeneticsoncology.org/Anomalies/t1114ID2021.html. Accessed on: 10 August 2010.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 315. ISBN 978-1416054542.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 317. ISBN 978-1416054542.
- ↑ URL: http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=cmed&part=A34022&rendertype=table&id=A34029. Accessed on: 20 August 2010.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 318. ISBN 978-1416054542.
- ↑ Lamant L, Meggetto F, al Saati T, et al. (January 1996). "High incidence of the t(2;5)(p23;q35) translocation in anaplastic large cell lymphoma and its lack of detection in Hodgkin's disease. Comparison of cytogenetic analysis, reverse transcriptase-polymerase chain reaction, and P-80 immunostaining". Blood 87 (1): 284–91. PMID 8547653.