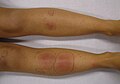
Panniculitis
Jump to navigation
Jump to search
Panniculitis is inflammation of the adipose tissue and fits into the larger category of inflammatory skin disorders. It is encountered in dermatopathology specimens.
Classification
- Lobular - involve fat lobules.
- Septal - involve interlobular septae.
A simple general DDx
Septal:
Lobular:
- Erythema induratum.
- Self-inflicted trauma (factitial panniculitis).
- Systemic lupus erythematosus.
- Other.
DDx by type
Septal:
- Erythema nodosum.
- Scleroderma panniculitis, also morphea profunda.[1]
Lobular:[1]
- Infectious panniculitis.
- Erythema induratum.
- Lupus panniculitis.
- Pancreatic panniculitis.
- Alpha1-antitrypsin deficiency.
- Subcutaneous fat necrosis of the newborn.
- Sclerema neonatorum.
Specific conditions
Erythema nodosum
General
Causes - mnemonic NODOSUM:[2]
- NO cause (idiopathic) ~ 55% of cases.
- Drugs (sulfonamides, amoxicillin, oral contraceptives) ~ 5% of cases.
- Other infections - group A streptococci (streptococcal pharyngitis), Yersinia, chlamydia, mycobacteria, others ~ 30% of cases.
- Sarcoidosis ~ 7% of cases.
- Ulcerative colitis & Crohn's disease ~ 2% of cases.
- Malignancy (leukemia, Hodgkin's lymphoma) ~ 1% of cases
Clinical:[4]
- Painful.
- Tender.
- Sudden onset.
- Heal without scarring.
Gross
Microscopic
- Expanded septa between fat lobules - key (low power) feature.
- Neutrophils.
- Lymphocytes.
- Histiocytes.
- Fibrin.
Notes:
- No vasculitis.
- +/-Granulomas - within the septa.[8]
- No ulceration.[4]
DDx:
Images
Morphea profunda
- AKA scleroderma panniculitis.
Main article: Morphea profunda
Erythema induratum
General
Features:[6]
- Uncommon.
- Etiology: unknown.
- Brinster[1] suggests an association, in some cases, with Mycobacterium tuberculosis and hepatitis C.
Clinical:[7]
- Classic location: posterior shins.
- Ulcerates and scars.
Microscopic
Features:[6]
- Predominantly lobular process with:[3]
- Necrotizing granulomatous inflammation.
- Necrotizing vasculitis of small/medium sized vessels (early).
DDx:
- Granulomatous infection.
- Vasculitis.
Images:
Stains
- AFB stain - exclude Tuberculosis.
See also
References
- ↑ 1.0 1.1 1.2 Brinster, NK. (Nov 2008). "Dermatopathology for the surgical pathologist: a pattern-based approach to the diagnosis of inflammatory skin disorders (part II).". Adv Anat Pathol 15 (6): 350-69. doi:10.1097/PAP.0b013e31818b1ac6. PMID 18948765.
- ↑ 2.0 2.1 Schwartz, RA.; Nervi, SJ. (Mar 2007). "Erythema nodosum: a sign of systemic disease.". Am Fam Physician 75 (5): 695-700. PMID 17375516.
- ↑ 3.0 3.1 URL: http://www.medscape.com/viewarticle/440356_8. Accessed on: 11 September 2011.
- ↑ 4.0 4.1 4.2 4.3 Requena, L.; Requena, C. (Jun 2002). "Erythema nodosum.". Dermatol Online J 8 (1): 4. PMID 12165214.
- ↑ Babamahmoodi, F.; Babamahmoodi, A.; Barani, H.; Delavarian, L. (2012). "Simultaneous occurrence of erythema nodosum in monozygotic twin sisters.". Case Rep Med 2012: 109427. doi:10.1155/2012/109427. PMID 22719770.
- ↑ 6.0 6.1 6.2 Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1199. ISBN 978-1416031215.
- ↑ 7.0 7.1 Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 609. ISBN 978-1416054542.
- ↑ 8.0 8.1 URL: http://missinglink.ucsf.edu/lm/DermatologyGlossary/erythema_nodosum.html. Accessed on: 11 September 2011.