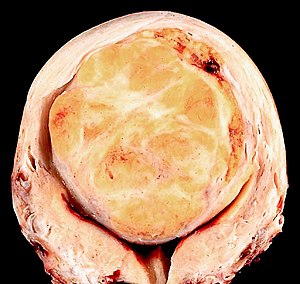
Hysterectomy for fibroids grossing
This protocol a protocol for grossing a hysterectomy for fibroids, also hysterectomy for leiomyomas.
It also covers grossing a hysterectomy for benign disease.
Introduction
This is a very common surgery. It said that approximately 40% of forty year old have fibroids. Other indications for hysterectomy are: dysfunctional uterine bleeding and hemorrhage (postpartum).
Unexpected malignancies (based on a series of 6,360 cases) are seen in approximately 2.7% of cases and include (1) endometrial carcinoma (1.02% of cases), (2) cancers of the tube, ovary and peritoneum (1.08% of cases), (3) uterine sarcoma (0.22% of cases), (4) metastatic disease (0.20% of cases) and (5) cervical cancer (0.17% of cases).[1]
In prophylatic procedures for BRCA1 mutation or BRCA2 mutation carriers, the ovaries and tubes, endometrium, and lower uterine segment should all be submitted in total.[2]
Opening
Orientation of hysterectomies
- Less peritoneum on anterior (as the urinary bladder is there).
- Posterior peritoneal edge: pointy (upside down triangle).
- Anterior peritoneal edge: rounded/non-pointy.
- Posterior peritoneal edge: pointy (upside down triangle).
- Tubes on anterior-lateral aspect.[3]
- Round ligaments posterior to tubes.
Protocol
Specimen type: total hysterectomy.
Dimensions:
- Uterus and cervix: ___x___x___cm, ____grams.
- Left ovary: ___x___x___cm.
- Left fallopian tube: length ___ cm, diameter ___cm.
- Right ovary: ___x___x___cm.
- Right fallopian tube: length ___ cm, diameter ____cm.
- Exocervix: diameter ___ cm.
Appearance:
- Uterine shape: pear-shaped/distorted.
- Serosal surface: smooth shiny.
- Serosa lesions: none/nodules up to ___cm in greatest dimension.
- Ectocervix: tan-white glistening with a probe patent os.
Internal dimensions:
- Endometrial cavity: ___x___cm.
- Endometrium: thickness ___cm.
- Maximal myometrial wall thickness: ___cm.
- Endocervical canal: length ___ cm, diameter ___ cm.
Internal/additional appearance:
- Left ovary: unremarkable.
- Left fallopian tube: unremarkable.
- Right ovary: unremarkable.
- Right fallopian tube: unremarkable.
Tumour(s):
- Appearance and location: intramural and subserosal white, firm, and whorled circumscribed/ill defined nodules.
- Number of tumors: ___.
- Size: range ___to ___cm in greatest dimension.
- Hemorrhage: present in ___ % of tumor / absent.
- Necrosis: present in ___ % of tumor / absent.
- Calcification: present / absent.
Additional findings: ___.
SECTION CODE:
- Anterior cervix and lower uterine segment
- Posterior cervix and lower uterine segment
- Posterior endomyometrium, full thickness
- Right ovary and , right fallopian tube [fimbria submitted entirely], with paratubal cysts
- Left ovary and left fallopian tube [fimbria submitted entirely]
- Submit sections of fibroids as per protocol (see next page).
Protocol notes
In prophylatic procedures for BRCA1 mutation or BRCA2 mutation carriers, the ovaries and tubes, endometrium, and lower uterine segment should all be submitted in total.[2]
Blocking protocol
Submit sections of fibroid as follows:
- Any suspicious areas of gross hemorrhage/ necrosis and softer consistency must be sampled.
- Any single fibroid >5 cm --> put one section per 2 cm, with put up to 2 sections per cassette.
- Any single fibroid >1 cm to up to 5 cm --> put one section per lesion
- Fibroids <=1 cm, and multiple in number --> use no more than five cassettes, each cassette can contain sections from two distinct fibroids.
- Any single fibroid >10 cm, please review the specimen with the attending pathologist.
Examples:
- 5.5 cm = 3 sections.
- 6 cm = 3 sections.
- 8 cm = 4 sections.
- 8 fibroids, all less than 1 cm = 4 cassettes, 2 sections per cassette.
- 15 fibroids = 5 cassettes, sample ten individual fibroids.
Alternate approaches
Also submit:
- Anterior endomyometrium, full thickness.
Do not submit:
- Posterior endomyometrium, full thickness.
See also
Related protocols
References
- ↑ Mahnert, N.; Morgan, D.; Campbell, D.; Johnston, C.; As-Sanie, S. (Feb 2015). "Unexpected gynecologic malignancy diagnosed after hysterectomy performed for benign indications.". Obstet Gynecol 125 (2): 397-405. doi:10.1097/AOG.0000000000000642. PMID 25569001.
- ↑ 2.0 2.1 Downes, MR.; Allo, G.; McCluggage, WG.; Sy, K.; Ferguson, SE.; Aronson, M.; Pollett, A.; Gallinger, S. et al. (Aug 2014). "Review of findings in prophylactic gynaecological specimens in Lynch syndrome with literature review and recommendations for grossing.". Histopathology 65 (2): 228-39. doi:10.1111/his.12386. PMID 24495259.
- ↑ Lester, Susan Carole (2010). Manual of Surgical Pathology (3rd ed.). Saunders. pp. 425. ISBN 978-0-323-06516-0.