Difference between revisions of "Ductal adenocarcinoma of the prostate gland"
Jump to navigation
Jump to search
(fix image) |
|||
| (3 intermediate revisions by the same user not shown) | |||
| Line 7: | Line 7: | ||
| Micro = | | Micro = | ||
| Subtypes = (subtype of [[prostate carcinoma]]) | | Subtypes = (subtype of [[prostate carcinoma]]) | ||
| LMDDx = [[acinar adenocarcinoma of prostate]], [[adenocarcinoma of the urinary bladder]], metastatic [[adenocarcinoma]] | | LMDDx = [[acinar adenocarcinoma of prostate]], [[prostatic-type polyp]], [[adenocarcinoma of the urinary bladder]], metastatic [[adenocarcinoma]] | ||
| Stains = | | Stains = | ||
| IHC = chromogranin A +ve, p53 +ve, PSA +ve | | IHC = chromogranin A +ve, p53 +ve, PSA +ve | ||
| EM = | | EM = | ||
| Molecular = | | Molecular = | ||
| Line 64: | Line 64: | ||
*[[Prostatic-type polyp]] - benign uncommon pathology, typically present with hematuria. | *[[Prostatic-type polyp]] - benign uncommon pathology, typically present with hematuria. | ||
*[[Adenocarcinoma of the urinary bladder]]. | *[[Adenocarcinoma of the urinary bladder]]. | ||
*[[PIN-like adenocarcinoma]] - does not have papillary architecture. | |||
*Metastatic [[adenocarcinoma]]. | *Metastatic [[adenocarcinoma]]. | ||
| Line 89: | Line 90: | ||
Others:<ref name=pmid20368883>{{Cite journal | last1 = Kumar | first1 = A. | last2 = Mukherjee | first2 = SD. | title = Metastatic ductal carcinoma of the prostate: a rare variant responding to a common treatment. | journal = Can Urol Assoc J | volume = 4 | issue = 2 | pages = E50-4 | month = Apr | year = 2010 | doi = | PMID = 20368883 }}</ref> | Others:<ref name=pmid20368883>{{Cite journal | last1 = Kumar | first1 = A. | last2 = Mukherjee | first2 = SD. | title = Metastatic ductal carcinoma of the prostate: a rare variant responding to a common treatment. | journal = Can Urol Assoc J | volume = 4 | issue = 2 | pages = E50-4 | month = Apr | year = 2010 | doi = | PMID = 20368883 }}</ref> | ||
*PSA +ve. | *PSA +ve. | ||
==Sign out== | |||
===Comment about small amount of ductal adenocarcinoma=== | |||
<pre> | |||
A small amount of ductal-type adenocarcinoma of the prostate is seen; it represents approximately 5% of the tumour by volume and is of no particular prognostic significance. As the volume of the ductal-type adenocarcinoma is small, the case is classified as acinar adenocarcinoma. | |||
</pre> | |||
==See also== | ==See also== | ||
Latest revision as of 14:46, 19 February 2019
Ductal adenocarcinoma of the prostate gland, also prostatic ductal adenocarcinoma, is relatively common variant of prostate cancer.
| Ductal adenocarcinoma of the prostate gland | |
|---|---|
| Diagnosis in short | |
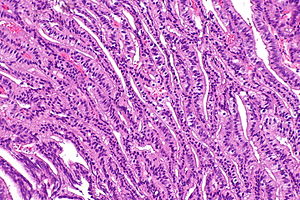 Ductal adenocarcinoma of prostate. H&E stain. (WC) | |
|
| |
| Synonyms | prostatic ductal adenocarcinoma, endometrioid adenocarcinoma (use discouraged), papillary adenocarcinoma of prostate (old term) |
| Subtypes | (subtype of prostate carcinoma) |
| LM DDx | acinar adenocarcinoma of prostate, prostatic-type polyp, adenocarcinoma of the urinary bladder, metastatic adenocarcinoma |
| IHC | chromogranin A +ve, p53 +ve, PSA +ve |
| Grossing notes | prostate biopsy, prostate chips, radical prostatectomy |
| Staging | prostate cancer staging |
| Site | prostate gland - esp. central zone, see prostate cancer |
|
| |
| Prevalence | uncommon - though considered most common non-acinar prostate carcinoma |
| Prognosis | poor |
It is also known as prostatic adenocarcinoma, large duct type.
It should not be confused with intraductal carcinoma of the prostate gland.
General
- Sometimes it is referred to as endometrioid or endometrial adenocarcinoma; both terms are discouraged.[1]
- In older literature it is referred to as papillary adenocarcinoma of the prostate.[2][3]
- Not completely uncontroversial - may represent acinar adenocarcinoma with periurethral ducts involvement.[4]
- More aggressive than conventional (acinar) prostate carcinoma.
Microscopic
Features:[5]
- Pseudostratified (crowded appearing) columnar (or cigar-shaped) nuclei - key feature.
- Vaguely resembles colonic adenocarcinoma.
- Compatible architecture:
- Papillary.
- Cribriform.
- Single gland (large glands).
- Endometrioid - vaguely looks like endometrioid endometrial carcinoma (with back-to-back glands).
- >= 50% of tumour.[6] ‡‡
- If ductal component <50%, it is a conventional (acinar) adenocarcinoma with a ductal component.
Notes:
- Proportion of ductal component should be quantified:
- <10% ductal component of no prognostic significance.[6]
- ‡‡ Mahul Amin advocates that >=80% should be ductal morphology to call ductal adenocarcinoma.[7]
DDx:
- Acinar adenocarcinoma of prostate - main DDx.
- Prostatic-type polyp - benign uncommon pathology, typically present with hematuria.
- Adenocarcinoma of the urinary bladder.
- PIN-like adenocarcinoma - does not have papillary architecture.
- Metastatic adenocarcinoma.
Images
www
- Prostatic ductal adenocarcinoma - several images (upmc.edu).
- Prostatic ductal adenocarcinoma - another case - several images (upmc.edu).
- Prostatic ductal adenocarcinoma - F1 (nih.gov).
- Prostatic ductal adenocarcinoma - F2 (nih.gov).
- Prostatic ductal adenocarcinoma (webpathology.com).
- Prostatic ductal adenocarcinoma (webpathology.com).
IHC
Features:[8]
- p53 +ve in ~ 75% of cases.
- Ki-67 high in ~ 70% of cases.
- Chromogranin A +ve (cytoplasm) in ~ 70% of cases.
Others:[9]
- PSA +ve.
Sign out
Comment about small amount of ductal adenocarcinoma
A small amount of ductal-type adenocarcinoma of the prostate is seen; it represents approximately 5% of the tumour by volume and is of no particular prognostic significance. As the volume of the ductal-type adenocarcinoma is small, the case is classified as acinar adenocarcinoma.
See also
References
- ↑ Samaratunga, H.; Delahunt, B. (Aug 2008). "Ductal adenocarcinoma of the prostate: current opinion and controversies.". Anal Quant Cytol Histol 30 (4): 237-46. PMID 18773743.
- ↑ Miki, J.; Ikemoto, I.; Shimomura, T.; Kiyota, H.; Oisi, Y.; Kondo, I.; Madarame, J.; Endo, K. et al. (Jan 2003). "[Papillary adenocarcinoma of the prostate: report of 4 cases].". Hinyokika Kiyo 49 (1): 21-4. PMID 12629776.
- ↑ Wernert, N.; Lüchtrath, H.; Seeliger, H.; Schäfer, M.; Goebbels, R.; Dhom, G. (1987). "Papillary carcinoma of the prostate, location, morphology, and immunohistochemistry: the histogenesis and entity of so-called endometrioid carcinoma.". Prostate 10 (2): 123-31. PMID 2436204.
- ↑ Bock, BJ.; Bostwick, DG. (Jul 1999). "Does prostatic ductal adenocarcinoma exist?". Am J Surg Pathol 23 (7): 781-5. PMID 10403300.
- ↑ Zhou, Ming; Magi-Galluzzi, Cristina (2006). Genitourinary Pathology: A Volume in Foundations in Diagnostic Pathology Series (1st ed.). Churchill Livingstone. pp. 88. ISBN 978-0443066771.
- ↑ 6.0 6.1 Amin, A.; Epstein, JI. (Apr 2011). "Pathologic stage of prostatic ductal adenocarcinoma at radical prostatectomy: effect of percentage of the ductal component and associated grade of acinar adenocarcinoma.". Am J Surg Pathol 35 (4): 615-9. doi:10.1097/PAS.0b013e31820eb25b. PMID 21383610.
- ↑ Amin, Mahul B. (2010). Diagnostic Pathology: Genitourinary (1st ed.). Amirsys. pp. 3-102. ISBN 978-1931884280.
- ↑ Tarján, M.; Lenngren, A.; Hellberg, D.; Tot, T. (Jun 2012). "Immunohistochemical verification of ductal differentiation in prostate cancer.". APMIS 120 (6): 510-8. doi:10.1111/j.1600-0463.2011.02862.x. PMID 22583364.
- ↑ Kumar, A.; Mukherjee, SD. (Apr 2010). "Metastatic ductal carcinoma of the prostate: a rare variant responding to a common treatment.". Can Urol Assoc J 4 (2): E50-4. PMID 20368883.