Difference between revisions of "Sertoli-Leydig cell tumour"
(→General: +DICER) |
|||
| (42 intermediate revisions by 2 users not shown) | |||
| Line 3: | Line 3: | ||
==General== | ==General== | ||
*Sertoli and leydig cells are normal in the [[testis]]. | *Sertoli and leydig cells are normal in the [[testis]]. | ||
* | **Tumor was called androblastoma or arrhenoblastoma in the past | ||
*May present with masculinization (virilization).<ref name=pmid23173550>{{Cite journal | last1 = Xiao | first1 = H. | last2 = Li | first2 = B. | last3 = Zuo | first3 = J. | last4 = Feng | first4 = X. | last5 = Li | first5 = X. | last6 = Zhang | first6 = R. | last7 = Wu | first7 = L. | title = Ovarian Sertoli-Leydig cell tumor: a report of seven cases and a review of the literature. | journal = Gynecol Endocrinol | volume = 29 | issue = 3 | pages = 192-5 | month = Mar | year = 2013 | doi = 10.3109/09513590.2012.738723 | PMID = 23173550 }}</ref> | *May present with masculinization (virilization).<ref name=pmid23173550>{{Cite journal | last1 = Xiao | first1 = H. | last2 = Li | first2 = B. | last3 = Zuo | first3 = J. | last4 = Feng | first4 = X. | last5 = Li | first5 = X. | last6 = Zhang | first6 = R. | last7 = Wu | first7 = L. | title = Ovarian Sertoli-Leydig cell tumor: a report of seven cases and a review of the literature. | journal = Gynecol Endocrinol | volume = 29 | issue = 3 | pages = 192-5 | month = Mar | year = 2013 | doi = 10.3109/09513590.2012.738723 | PMID = 23173550 }}</ref> | ||
*May present as abdominal swelling or pain. | |||
*Generally a tumor of younger women and can present in children.<ref>{{Cite journal | last1 = Young | first1 = RH. | last2 = Scully | first2 = RE. | title = Ovarian Sertoli-Leydig cell tumors. A clinicopathological analysis of 207 cases. | journal = Am J Surg Pathol | volume = 9 | issue = 8 | pages = 543-69 | month = Aug | year = 1985 | doi = | PMID = 3911780 }}</ref> | |||
**75% younger than 30 years of age | |||
**10% over 50 years of age. | |||
*[[DICER1 mutation]] common in moderately and poorly differentiated Sertoli-Leydig cell tumours.<ref name=pmid28654427>{{Cite journal | last1 = de Kock | first1 = L. | last2 = Terzic | first2 = T. | last3 = McCluggage | first3 = WG. | last4 = Stewart | first4 = CJR. | last5 = Shaw | first5 = P. | last6 = Foulkes | first6 = WD. | last7 = Clarke | first7 = BA. | title = DICER1 Mutations Are Consistently Present in Moderately and Poorly Differentiated Sertoli-Leydig Cell Tumors. | journal = Am J Surg Pathol | volume = 41 | issue = 9 | pages = 1178-1187 | month = Sep | year = 2017 | doi = 10.1097/PAS.0000000000000895 | PMID = 28654427 }}</ref> | |||
==Microscopic== | ==Microscopic== | ||
Features: | Features: | ||
* Sertoli ''or'' Leydig cells.<ref name=Ref_PBoD1103>{{Ref PBoD|1103}}</ref> | |||
** Leydig cells: | |||
***Polygonal pink cells | |||
*** Abundant solid or somewhat granular eosinophilic cytoplasm. | |||
*** Round nuclei with fine chromatin and a small or indistinct [[nucleolus]]. | |||
*** Often in small clusters ~ 5-25 cells/cluster. | |||
** Sertoli cells: | |||
*** Pale/clear vacuolated cytoplasm. | |||
*** Irregular nuclei with irregular/vacuolated-appearing chromatin. | |||
*** Architecture: tubules, cords or sheets. | |||
****Classic Sertoli tubule shows an 'antipodal arrangement of nuclei' | |||
*****Nuclei sit near the basement membrane away from the tubule lumen. | |||
*****A fair bit of cytoplasm sits above the nucleus. | |||
*****Lumen is round. | |||
***Mitotic activity may be much lower than expected for the degree of atypia (in comparison to adenocarcinoma). | |||
**Stroma | |||
***Varies from fibrous pink stroma in well differentiated tumors to cellular primative stroma in poorly differentiated tumors. | |||
***+/-Stromal edema may be prominent | |||
*Growth Patterns: | |||
**Well-differentiated. | |||
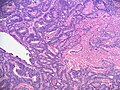
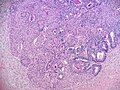
***Hollow or solid tubules of mature Sertoli cells with Leydig cells in the intervening stroma. | |||
**Intermediate (most common). | |||
***Jumbled admixture of dark blue Sertoli cells and Leydig cells. | |||
***Lobules comprising sheets of Sertoli cells. | |||
***Some areas of tubules. | |||
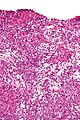
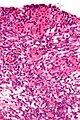
**Poorly differentiated. | |||
***Masses of malignant spindle cells – sheets of cells can be reminiscent of fibrosarcoma or granulosa cell tumour. | |||
***Tubules may be a very minor element. | |||
***Poorly differentiated tumours have sarcomatous features.<ref name=Ref_PBoD1103>{{Ref PBoD|1103}}</ref> | |||
**Retiform.<ref>{{Cite journal | last1 = Young | first1 = RH. | last2 = Scully | first2 = RE. | title = Ovarian Sertoli-Leydig cell tumors with a retiform pattern: a problem in histopathologic diagnosis. A report of 25 cases. | journal = Am J Surg Pathol | volume = 7 | issue = 8 | pages = 755-71 | month = Dec | year = 1983 | doi = | PMID = 6660351 }}</ref> | |||
***Tumour resembles rete testis/ovary with an irregular network of elongated slit-like tubules and cysts, which may contain papillae. | |||
**With heterologous element. | |||
***Mucinous intestinal-type epithelium, cartilage, skeletal muscle. | |||
***Heterologous elements can occur in retiform or poorly differentiated tumours. | |||
***+/-Sarcomatous features (mucinous glands, bone, cartilage). | |||
DDx: | DDx: | ||
*[[Endometrioid carcinoma of the ovary]]. | *[[Endometrioid carcinoma of the ovary]] (sertoliform variant) | ||
*Luteinized [[adult granulosa cell tumour]] - super rare, 50% of cell with eosinophilic cytoplasm, other findings of granulosa cell tumour, e.g. Call-Exner bodies.<ref name=pmid21804396>{{Cite journal | last1 = Ganesan | first1 = R. | last2 = Hirschowitz | first2 = L. | last3 = Baltrušaitytė | first3 = I. | last4 = McCluggage | first4 = WG. | title = Luteinized adult granulosa cell tumor--a series of 9 cases: revisiting a rare variant of adult granulosa cell tumor. | journal = Int J Gynecol Pathol | volume = 30 | issue = 5 | pages = 452-9 | month = Sep | year = 2011 | doi = 10.1097/PGP.0b013e318214b17f | PMID = 21804396 }}</ref> | **Should be positive for EMA, CK7 and negative for inhibin and calretinin.<ref>{{Cite journal | last1 = McCluggage | first1 = WG. | last2 = Young | first2 = RH. | title = Ovarian sertoli-leydig cell tumors with pseudoendometrioid tubules (pseudoendometrioid sertoli-leydig cell tumors). | journal = Am J Surg Pathol | volume = 31 | issue = 4 | pages = 592-7 | month = Apr | year = 2007 | doi = 10.1097/01.pas.0000213365.56498.72 | PMID = 17414107 }}</ref> | ||
**Should have some characteristic areas of endometriod carcinoma and may have some typical features | |||
***Cilia, squamous metaplasia, mucin production | |||
*Luteinized [[adult granulosa cell tumour]] - super rare, 50% of cell with eosinophilic cytoplasm, other findings of granulosa cell tumour, e.g. Call-Exner bodies. More likely to be keratin negative than a Sertoli-Leydig cell tumor. <ref name=pmid21804396>{{Cite journal | last1 = Ganesan | first1 = R. | last2 = Hirschowitz | first2 = L. | last3 = Baltrušaitytė | first3 = I. | last4 = McCluggage | first4 = WG. | title = Luteinized adult granulosa cell tumor--a series of 9 cases: revisiting a rare variant of adult granulosa cell tumor. | journal = Int J Gynecol Pathol | volume = 30 | issue = 5 | pages = 452-9 | month = Sep | year = 2011 | doi = 10.1097/PGP.0b013e318214b17f | PMID = 21804396 }}</ref> | |||
*Ovarian carcinosarcoma - especially considering poorly differentiated versions with heterologous areas. | |||
Retiform variant | |||
*Ovarian serous carcinoma - generally carcinoma patients are older. | |||
*Ovarian yolk sac tumor | |||
===Images=== | ===Images=== | ||
<gallery> | <gallery> | ||
| Line 36: | Line 67: | ||
Image:Sertoli-Leydig_cell_tumour_-_high_mag.jpg | Sertoli-Leydig cell tumour - high mag. (WC) | Image:Sertoli-Leydig_cell_tumour_-_high_mag.jpg | Sertoli-Leydig cell tumour - high mag. (WC) | ||
Image:Sertoli-Leydig_cell_tumour_-_very_high_mag.jpg | Sertoli-Leydig cell tumour - very high mag. (WC) | Image:Sertoli-Leydig_cell_tumour_-_very_high_mag.jpg | Sertoli-Leydig cell tumour - very high mag. (WC) | ||
Image:Ovary SertoliLeydigCellTumor 4 PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated - low power (SKB) | |||
Image:Ovary SertoliLeydigCellTumor 5 PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated - low power (SKB) | |||
Image:Ovary SertoliLeydigCellTumor 7 PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated - medium power (SKB) | |||
Image:Ovary SertoliLeydigCellTumor 6 PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated (SKB) | |||
Image:Ovary SertoliLeydigCellTumor.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated (SKB) | |||
Image:Ovary SertoliLeydigCellTumor 3 PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated - see how much cytoplasm is between the nucleus and the lumen? See the crisp outline of the lumen by the apical membrane of the cells - this is a typical Leydig tubule. (SKB) | |||
Image:Ovary SertoliLeydigCellTumor PA.jpg|Ovarian Sertoli Leydig Cell Tumor - Well differentiated (SKB) | |||
Image:Ovary SertoliLeydigCellTumor MP2 CTR.jpg|Ovarian Sertoli Leydig Cell Tumor - medium power - This example is somewhat between the previous well differentiated and following intermediate differentiated examples (SKB) | |||
Image:Ovary SertoliLeydigCellTumor MP3 CTR.jpg|Ovarian Sertoli Leydig Cell Tumor - medium power (SKB) | |||
Image:Ovary SertoliLeydigCellTumor MP CTR.jpg|Ovarian Sertoli Leydig Cell Tumor - medium power (SKB) | |||
Image:Ovary SertoliLeydig Intermediate MP CTR.jpg|Ovarian Sertoli-Leydig Cell Tumor - Intermediate differentiation - Medium power (SKB) | |||
Image:Ovary SertoliLeydig Intermediate HP CTR.jpg|Ovarian Sertoli-Leydig Cell Tumor - Intermediate differentiation - High power (SKB) | |||
Image:Ovary SertoliLeydig Intermediate HP2 CTR.jpg|Ovarian Sertoli-Leydig Cell Tumor - Intermediate differentiation - High power (SKB) | |||
</gallery> | </gallery> | ||
www: | www: | ||
*[http://path.upmc.edu/cases/case270/micro.html Sex cord stromal tumour with Sertoli-Leydig component - several images (upmc.edu)]. | *[http://path.upmc.edu/cases/case270/micro.html Sex cord stromal tumour with Sertoli-Leydig component - several images (upmc.edu)]. | ||
==Prognosis== | |||
*Dependant on degree of differentiation and stage at presentation.<ref>{{Cite journal | last1 = Young | first1 = RH. | last2 = Scully | first2 = RE. | title = Ovarian Sertoli-Leydig cell tumors. A clinicopathological analysis of 207 cases. | journal = Am J Surg Pathol | volume = 9 | issue = 8 | pages = 543-69 | month = Aug | year = 1985 | doi = | PMID = 3911780 }}</ref> | |||
*Heterologous mesenchymal elements may portend a worse outcome.<ref>{{Cite journal | last1 = Zaloudek | first1 = C. | last2 = Norris | first2 = HJ. | title = Sertoli-Leydig tumors of the ovary. A clinicopathologic study of 64 intermediate and poorly differentiated neoplasms. | journal = Am J Surg Pathol | volume = 8 | issue = 6 | pages = 405-18 | month = Jun | year = 1984 | doi = | PMID = 6731664 }}</ref> | |||
==IHC== | ==IHC== | ||
Features:<ref name=pmid19033865>{{Cite journal | last1 = Zhao | first1 = C. | last2 = Vinh | first2 = TN. | last3 = McManus | first3 = K. | last4 = Dabbs | first4 = D. | last5 = Barner | first5 = R. | last6 = Vang | first6 = R. | title = Identification of the most sensitive and robust immunohistochemical markers in different categories of ovarian sex cord-stromal tumors. | journal = Am J Surg Pathol | volume = 33 | issue = 3 | pages = 354-66 | month = Mar | year = 2009 | doi = 10.1097/PAS.0b013e318188373d | PMID = 19033865 }}</ref> | Features:<ref name=pmid19033865>{{Cite journal | last1 = Zhao | first1 = C. | last2 = Vinh | first2 = TN. | last3 = McManus | first3 = K. | last4 = Dabbs | first4 = D. | last5 = Barner | first5 = R. | last6 = Vang | first6 = R. | title = Identification of the most sensitive and robust immunohistochemical markers in different categories of ovarian sex cord-stromal tumors. | journal = Am J Surg Pathol | volume = 33 | issue = 3 | pages = 354-66 | month = Mar | year = 2009 | doi = 10.1097/PAS.0b013e318188373d | PMID = 19033865 }}</ref> | ||
* | |||
* | *'''Inhibin''' +ve | ||
*'''Calretinin''' +ve. | |||
*WT-1 +ve. | *WT-1 +ve. | ||
*Melan A (MART-1) +ve - marks the Leydig component. | *Melan A (MART-1) +ve - marks the Leydig component. | ||
*Vimentin +ve.<ref name=pmid20349790>{{Cite journal | last1 = Kondi-Pafiti | first1 = A. | last2 = Grapsa | first2 = D. | last3 = Kairi-Vassilatou | first3 = E. | last4 = Carvounis | first4 = E. | last5 = Hasiakos | first5 = D. | last6 = Kontogianni | first6 = K. | last7 = Fotiou | first7 = S. | title = Granulosa cell tumors of the ovary: a clinicopathologic and immunohistochemical study of 21 cases. | journal = Eur J Gynaecol Oncol | volume = 31 | issue = 1 | pages = 94-8 | month = | year = 2010 | doi = | PMID = 20349790 }}</ref> | *Vimentin +ve.<ref name=pmid20349790>{{Cite journal | last1 = Kondi-Pafiti | first1 = A. | last2 = Grapsa | first2 = D. | last3 = Kairi-Vassilatou | first3 = E. | last4 = Carvounis | first4 = E. | last5 = Hasiakos | first5 = D. | last6 = Kontogianni | first6 = K. | last7 = Fotiou | first7 = S. | title = Granulosa cell tumors of the ovary: a clinicopathologic and immunohistochemical study of 21 cases. | journal = Eur J Gynaecol Oncol | volume = 31 | issue = 1 | pages = 94-8 | month = | year = 2010 | doi = | PMID = 20349790 }}</ref> | ||
*CD99 +ve. | *CD99 +ve. | ||
*[[AE1/AE3]] and [[pankeratin]] +ve | |||
Others:<ref name=pmid20349790/> | Others:<ref name=pmid20349790/> | ||
*CD34 -ve. | *CD34 -ve. | ||
*EMA -ve. | *'''[[EMA]]''' -ve. | ||
*[[CK7]] -ve. | |||
Keep in mind that this is a biphasic tumor - Leydig cells will not be Pan-keratin positive - Sertoli cells do not express calretinin - Both components express inhibin - etcetera - interpreting this immunopanal requires correlation with the histomorphology. Immunoreactivity may be focal. | |||
Pan-keratins and AE1/AE3 may mark granulosa cell tumors and Sertoli cell tumors causing confusion with adenocarcinoma. EMA is a better marker to exclude an epithelial tumor as EMA is negative in sex cord-stromal tumors. | Pan-keratins and AE1/AE3 may mark granulosa cell tumors and Sertoli cell tumors causing confusion with adenocarcinoma. EMA is a better marker to exclude an epithelial tumor as EMA is negative in sex cord-stromal tumors. Highlighting why a panel of stains is needed, endometrioid adenocarcinomas may occasionally weakly express inhibin, calretinin or WT-1. | ||
==See also== | ==See also== | ||
Latest revision as of 09:43, 11 September 2018
Sertoli-Leydig cell tumour, also Sertoli-Leydig tumour, is a rare tumour of the gonad in the sex cord-stromal group of tumours.
General
- Sertoli and leydig cells are normal in the testis.
- Tumor was called androblastoma or arrhenoblastoma in the past
- May present with masculinization (virilization).[1]
- May present as abdominal swelling or pain.
- Generally a tumor of younger women and can present in children.[2]
- 75% younger than 30 years of age
- 10% over 50 years of age.
- DICER1 mutation common in moderately and poorly differentiated Sertoli-Leydig cell tumours.[3]
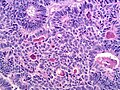
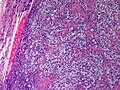
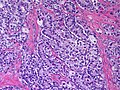
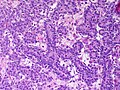
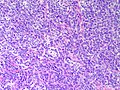
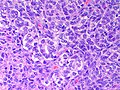
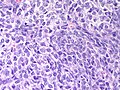
Microscopic
Features:
- Sertoli or Leydig cells.[4]
- Leydig cells:
- Polygonal pink cells
- Abundant solid or somewhat granular eosinophilic cytoplasm.
- Round nuclei with fine chromatin and a small or indistinct nucleolus.
- Often in small clusters ~ 5-25 cells/cluster.
- Sertoli cells:
- Pale/clear vacuolated cytoplasm.
- Irregular nuclei with irregular/vacuolated-appearing chromatin.
- Architecture: tubules, cords or sheets.
- Classic Sertoli tubule shows an 'antipodal arrangement of nuclei'
- Nuclei sit near the basement membrane away from the tubule lumen.
- A fair bit of cytoplasm sits above the nucleus.
- Lumen is round.
- Classic Sertoli tubule shows an 'antipodal arrangement of nuclei'
- Mitotic activity may be much lower than expected for the degree of atypia (in comparison to adenocarcinoma).
- Stroma
- Varies from fibrous pink stroma in well differentiated tumors to cellular primative stroma in poorly differentiated tumors.
- +/-Stromal edema may be prominent
- Leydig cells:
- Growth Patterns:
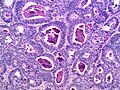
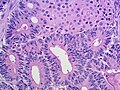
- Well-differentiated.
- Hollow or solid tubules of mature Sertoli cells with Leydig cells in the intervening stroma.
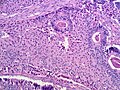
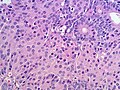
- Intermediate (most common).
- Jumbled admixture of dark blue Sertoli cells and Leydig cells.
- Lobules comprising sheets of Sertoli cells.
- Some areas of tubules.
- Poorly differentiated.
- Masses of malignant spindle cells – sheets of cells can be reminiscent of fibrosarcoma or granulosa cell tumour.
- Tubules may be a very minor element.
- Poorly differentiated tumours have sarcomatous features.[4]
- Retiform.[5]
- Tumour resembles rete testis/ovary with an irregular network of elongated slit-like tubules and cysts, which may contain papillae.
- With heterologous element.
- Mucinous intestinal-type epithelium, cartilage, skeletal muscle.
- Heterologous elements can occur in retiform or poorly differentiated tumours.
- +/-Sarcomatous features (mucinous glands, bone, cartilage).
- Well-differentiated.
DDx:
- Endometrioid carcinoma of the ovary (sertoliform variant)
- Should be positive for EMA, CK7 and negative for inhibin and calretinin.[6]
- Should have some characteristic areas of endometriod carcinoma and may have some typical features
- Cilia, squamous metaplasia, mucin production
- Luteinized adult granulosa cell tumour - super rare, 50% of cell with eosinophilic cytoplasm, other findings of granulosa cell tumour, e.g. Call-Exner bodies. More likely to be keratin negative than a Sertoli-Leydig cell tumor. [7]
- Ovarian carcinosarcoma - especially considering poorly differentiated versions with heterologous areas.
Retiform variant
- Ovarian serous carcinoma - generally carcinoma patients are older.
- Ovarian yolk sac tumor
Images
www:
Prognosis
- Dependant on degree of differentiation and stage at presentation.[8]
- Heterologous mesenchymal elements may portend a worse outcome.[9]
IHC
Features:[10]
- Inhibin +ve
- Calretinin +ve.
- WT-1 +ve.
- Melan A (MART-1) +ve - marks the Leydig component.
- Vimentin +ve.[11]
- CD99 +ve.
- AE1/AE3 and pankeratin +ve
Others:[11]
Keep in mind that this is a biphasic tumor - Leydig cells will not be Pan-keratin positive - Sertoli cells do not express calretinin - Both components express inhibin - etcetera - interpreting this immunopanal requires correlation with the histomorphology. Immunoreactivity may be focal.
Pan-keratins and AE1/AE3 may mark granulosa cell tumors and Sertoli cell tumors causing confusion with adenocarcinoma. EMA is a better marker to exclude an epithelial tumor as EMA is negative in sex cord-stromal tumors. Highlighting why a panel of stains is needed, endometrioid adenocarcinomas may occasionally weakly express inhibin, calretinin or WT-1.
See also
References
- ↑ Xiao, H.; Li, B.; Zuo, J.; Feng, X.; Li, X.; Zhang, R.; Wu, L. (Mar 2013). "Ovarian Sertoli-Leydig cell tumor: a report of seven cases and a review of the literature.". Gynecol Endocrinol 29 (3): 192-5. doi:10.3109/09513590.2012.738723. PMID 23173550.
- ↑ Young, RH.; Scully, RE. (Aug 1985). "Ovarian Sertoli-Leydig cell tumors. A clinicopathological analysis of 207 cases.". Am J Surg Pathol 9 (8): 543-69. PMID 3911780.
- ↑ de Kock, L.; Terzic, T.; McCluggage, WG.; Stewart, CJR.; Shaw, P.; Foulkes, WD.; Clarke, BA. (Sep 2017). "DICER1 Mutations Are Consistently Present in Moderately and Poorly Differentiated Sertoli-Leydig Cell Tumors.". Am J Surg Pathol 41 (9): 1178-1187. doi:10.1097/PAS.0000000000000895. PMID 28654427.
- ↑ 4.0 4.1 Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Nelso Fausto; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease (7th ed.). St. Louis, Mo: Elsevier Saunders. pp. 1103. ISBN 0-7216-0187-1.
- ↑ Young, RH.; Scully, RE. (Dec 1983). "Ovarian Sertoli-Leydig cell tumors with a retiform pattern: a problem in histopathologic diagnosis. A report of 25 cases.". Am J Surg Pathol 7 (8): 755-71. PMID 6660351.
- ↑ McCluggage, WG.; Young, RH. (Apr 2007). "Ovarian sertoli-leydig cell tumors with pseudoendometrioid tubules (pseudoendometrioid sertoli-leydig cell tumors).". Am J Surg Pathol 31 (4): 592-7. doi:10.1097/01.pas.0000213365.56498.72. PMID 17414107.
- ↑ Ganesan, R.; Hirschowitz, L.; Baltrušaitytė, I.; McCluggage, WG. (Sep 2011). "Luteinized adult granulosa cell tumor--a series of 9 cases: revisiting a rare variant of adult granulosa cell tumor.". Int J Gynecol Pathol 30 (5): 452-9. doi:10.1097/PGP.0b013e318214b17f. PMID 21804396.
- ↑ Young, RH.; Scully, RE. (Aug 1985). "Ovarian Sertoli-Leydig cell tumors. A clinicopathological analysis of 207 cases.". Am J Surg Pathol 9 (8): 543-69. PMID 3911780.
- ↑ Zaloudek, C.; Norris, HJ. (Jun 1984). "Sertoli-Leydig tumors of the ovary. A clinicopathologic study of 64 intermediate and poorly differentiated neoplasms.". Am J Surg Pathol 8 (6): 405-18. PMID 6731664.
- ↑ Zhao, C.; Vinh, TN.; McManus, K.; Dabbs, D.; Barner, R.; Vang, R. (Mar 2009). "Identification of the most sensitive and robust immunohistochemical markers in different categories of ovarian sex cord-stromal tumors.". Am J Surg Pathol 33 (3): 354-66. doi:10.1097/PAS.0b013e318188373d. PMID 19033865.
- ↑ 11.0 11.1 Kondi-Pafiti, A.; Grapsa, D.; Kairi-Vassilatou, E.; Carvounis, E.; Hasiakos, D.; Kontogianni, K.; Fotiou, S. (2010). "Granulosa cell tumors of the ovary: a clinicopathologic and immunohistochemical study of 21 cases.". Eur J Gynaecol Oncol 31 (1): 94-8. PMID 20349790.