Difference between revisions of "Hodgkin lymphoma"
(tweak) |
m (fill in BCL6 and MUM1 in comparison table) |
||
| (13 intermediate revisions by 2 users not shown) | |||
| Line 18: | Line 18: | ||
| Assdx = | | Assdx = | ||
| Syndromes = | | Syndromes = | ||
| Clinicalhx = young adults, older | | Clinicalhx = young adults, older adults (bimodal distribution) | ||
| Signs = lymphadenopathy - usu. neck, +/-[[B symptoms]] (fever, night sweats, weight loss) | | Signs = lymphadenopathy - usu. neck, +/-[[B symptoms]] (fever, night sweats, weight loss) | ||
| Symptoms = | | Symptoms = | ||
| Line 29: | Line 29: | ||
| ClinDDx = | | ClinDDx = | ||
}} | }} | ||
'''Hodgkin [[lymphoma]]''', abbreviated '''HL''', is a haematological [[malignancy]]. If not otherwise specified, Hodgkin lymphoma generally refers to classical Hodgkin lymphoma (CHL) rather than [[nodular lymphocyte-predominant Hodgkin lymphoma]] (NLPHL). The latter accounts for only about 5% of the loose label of Hodgkin lymphoma<ref name=Ref_WMSP567/> and shows a sufficiently different biology and immunophenotype that is essentially a different disease (see [[nodular lymphocyte-predominant Hodgkin lymphoma|main article on NLPHL]]). The common feature is large atypical cells: Hodgkin/Reed-Sternberg cells in the case of classical Hodgkin lymphoma and "popcorn"/lymphohistiocytic/L&H cells in NLPHL. However, at least in typical cases, there are morphological and immunophenotypic differences. | |||
Classical Hodgkin lymphoma has a bi-modal distribution, afflicting young adults and with a further peak in incidence in middle-age. Fortunately, it usually has a good prognosis. | |||
Pathologists say "... it is both the easiest and hardest diagnosis to make." The reason for this is: the diagnosis depends on finding Reed-Sternberg cells; if they are obvious the diagnosis is easy... if you can't find 'em and an alternative diagnosis is not apparent -- you wonder whether you're missing them. | Pathologists say "... it is both the easiest and hardest diagnosis to make." The reason for this is: the diagnosis depends on finding Reed-Sternberg cells (or Popcorn cells); if they are obvious the diagnosis is easy... if you can't find 'em and an alternative diagnosis is not apparent -- you wonder whether you're missing them. | ||
==General== | ==General== | ||
| Line 75: | Line 47: | ||
*Usually good. | *Usually good. | ||
*Unlike non-Hodgkin lymphomas, it spreads in a predictable pattern; thus, staging plays an important role in determining the therapy.<ref name=PCPBoD8_315>{{Ref PCPBoD8|315}}</ref> | *Unlike non-Hodgkin lymphomas, it spreads in a predictable pattern; thus, staging plays an important role in determining the therapy.<ref name=PCPBoD8_315>{{Ref PCPBoD8|315}}</ref> | ||
*Clinically classified into early favourable, early unfavourable and late/advanced disease. | |||
== | ===Classic HL sub-types=== | ||
====Subtypes of classic HL==== | ====Subtypes of classic HL==== | ||
There are four CHL subtypes:<ref name=Ref_WMSP567/> | There are four CHL subtypes:<ref name=Ref_WMSP567/> | ||
| Line 133: | Line 66: | ||
*The subtypes prevalence is in reverse alphabetical order. | *The subtypes prevalence is in reverse alphabetical order. | ||
== | ==Gross== | ||
Location: | |||
*'' | *Almost always arises from a [[lymph node]] - classically in the neck, but may be in the axilla and mediastinum | ||
* | *Spleen may be involved | ||
** | *Bone marrow involvement is unusual (~5% of cases, higher in HIV-associated cases), so bone marrow assessment is usually not performed | ||
** | *''Extranodal Hodgkin lymphoma'' is (case report) rare.<ref name=pmid11100066>{{Cite journal | last1 = Vadmal | first1 = MS. | last2 = LaValle | first2 = GP. | last3 = DeYoung | first3 = BR. | last4 = Frankel | first4 = WL. | last5 = Marsh | first5 = WL. | title = Primary localized extranodal hodgkin disease of the transverse colon. | journal = Arch Pathol Lab Med | volume = 124 | issue = 12 | pages = 1824-7 | month = Dec | year = 2000 | doi = 10.1043/0003-9985(2000)1241824:PLEHDO2.0.CO;2 | PMID = 11100066 }}</ref> | ||
* | |||
==Microscopic== | |||
Defined by ''Reed-Sternberg cells'' (RSCs). Morphologically similar mononuclear cells are known as Hodgkin cells. RSCs are: | |||
*Large binucleated cell (>= 45 micrometres).<ref name=Ref_PCPBoD8_329>{{Ref PCPBoD8|329}}</ref> | |||
**May be multinucleated. | |||
**May have a horseshoe-like shape. | |||
*[[Macronucleolus]] - approximately the size of a RBC (~8 micrometers). | |||
*Well-defined cell border. | |||
*Abundant cytoplasm. | |||
RSC may show peri-cellular clearing, making the cells appear within a space. These are called lacunar cells (as they are in a "lake"). Apoptotic RSC may show pyknotic nuclei and scant eosinophilic cytoplasm and are sometimes known as "mummified" cells. | |||
===Images (classic HL)=== | |||
<gallery> | <gallery> | ||
Image: | Image:CHL mummified cell x40.jpg | "Mummified" RSC. (WC) | ||
Image:CHL lacunar cell x40.jpg | "Lacunar cell". (WC) | |||
Image:16S14098 cHL multinucleate HRS cell x40c.jpg | Multinucleate RSC. (WC) | |||
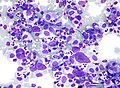
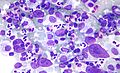
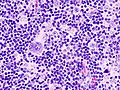
Image:Hodgkin_lymphoma_cytology_large.jpg | HL mixed cellularity - cytology. (WC) | |||
Image:Hodgkin_lymphoma_cytology_small.jpg | HL mixed cellularity - cytology. (WC) | |||
Image:Hodgkin_lymphoma_%281%29_mixed_cellulary_type.jpg | HL mixed cellularity. (WC) | |||
</gallery> | </gallery> | ||
===DDx both CHL & NLPHL=== | ===DDx both CHL & NLPHL=== | ||
*CHL/NLPHL. | *CHL/NLPHL. | ||
*[[Diffuse large B cell lymphoma]] (DLBCL), esp. ''T-cell/histiocytic-rich LBCL''. | *[[Diffuse large B cell lymphoma]] (DLBCL), esp. ''T-cell/histiocytic-rich LBCL''. | ||
*[[Anaplastic large cell lymphoma]] (ALCL). | *[[Anaplastic large cell lymphoma]] (ALCL). | ||
*B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma.<ref name=pmid22222636>{{Cite journal | last1 = Gualco | first1 = G. | last2 = Natkunam | first2 = Y. | last3 = Bacchi | first3 = CE. | title = The spectrum of B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma: a description of 10 cases. | journal = Mod Pathol | volume = | issue = | pages = | month = Jan | year = 2012 | doi = 10.1038/modpathol.2011.200 | PMID = 22222636 | URL = http://www.nature.com/modpathol/journal/vaop/ncurrent/full/modpathol2011200a.html }}</ref> | *B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma.<ref name=pmid22222636>{{Cite journal | last1 = Gualco | first1 = G. | last2 = Natkunam | first2 = Y. | last3 = Bacchi | first3 = CE. | title = The spectrum of B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma: a description of 10 cases. | journal = Mod Pathol | volume = | issue = | pages = | month = Jan | year = 2012 | doi = 10.1038/modpathol.2011.200 | PMID = 22222636 | URL = http://www.nature.com/modpathol/journal/vaop/ncurrent/full/modpathol2011200a.html }}</ref> (typically in cases of numerous large atypical cells where the morphology and immunophenotype do not neatly fit into either DLBCL or CHL). | ||
==IHC== | ==IHC== | ||
Abbreviated panel:<ref name=Ref_WMSP568>{{Ref_WMSP|568}}</ref> | Abbreviated panel:<ref name=Ref_WMSP568>{{Ref_WMSP|568}}</ref> | ||
*CD30 Reed-Sternberg cells (RSCs) +ve ~98% | *CD30 Reed-Sternberg cells (RSCs) +ve ~98% (beware of mis-interpreting CD30+ activated lymphoid cells) | ||
*CD15 Reed-Sternberg cells +ve ~80%, stains neutrophils. | *CD15 Reed-Sternberg cells +ve ~80%, stains neutrophils. | ||
*Both CD30 and CD15 are classically positive in a membranous and Golgi pattern | |||
*MUM1 +ve | |||
*CD45 '''often negative''' in RSCs. | *CD45 '''often negative''' in RSCs. | ||
*CD20 may stain RSCs. | *CD20 may stain RSCs (usually negative, but can be weak). | ||
*PAX5 +ve | *PAX5 +ve, though said to be weaker than background normal B-cells<ref name=Ref_APBR683>{{Ref APBR|683}}</ref> | ||
Additional - for completeness: | Additional - for completeness: | ||
*CD3 (T lymphocytes) | *CD3 (T lymphocytes) - negative in RSCs | ||
*OCT2/BOB1 negative (co-transcription factors for immunoglobulin production, one or the other is usually negative) | |||
*40% are EBV positive. | |||
NLPHL IHC '''differs''' from the classical HL:<ref name=Ref_APBR683>{{Ref APBR|683}}</ref> | NLPHL IHC '''differs''' from the classical HL:<ref name=Ref_APBR683>{{Ref APBR|683}}</ref> | ||
| Line 169: | Line 120: | ||
*CD10 +ve. | *CD10 +ve. | ||
*Bcl-6 +ve. | *Bcl-6 +ve. | ||
*EMA +ve | *[[EMA]] +ve (40-50%) | ||
*CD30 -ve | *CD30 -ve | ||
*CD15 -ve. | *CD15 -ve. | ||
=== | ===A panel=== | ||
{| class="wikitable" | {| class="wikitable" | ||
|Antibody || NLPHL || CHL | |Antibody || NLPHL || CHL | ||
| Line 181: | Line 132: | ||
|CD20 || +ve || -ve | |CD20 || +ve || -ve | ||
|- | |- | ||
|BCL6 || || | |BCL6 || +ve || -ve | ||
|- | |- | ||
|MUM1<ref>URL: [http://www.ncbi.nlm.nih.gov/omim/601900 http://www.ncbi.nlm.nih.gov/omim/601900]. Accessed on: 10 August 2010.</ref> || -ve || | |MUM1<ref>URL: [http://www.ncbi.nlm.nih.gov/omim/601900 http://www.ncbi.nlm.nih.gov/omim/601900]. Accessed on: 10 August 2010.</ref> || -ve || +ve | ||
|- | |- | ||
|CD30 || -ve || +ve (most sensitive). | |CD30 || -ve || +ve (most sensitive). | ||
| Line 191: | Line 142: | ||
|CD21 || networks present || no networks | |CD21 || networks present || no networks | ||
|- | |- | ||
|CD23 | |[[CD23]] || networks present || no networks | ||
|- | |- | ||
|OCT-2 || +ve || -ve | |OCT-2 || +ve || -ve | ||
| Line 207: | Line 158: | ||
|4 unstained || || | |4 unstained || || | ||
|} | |} | ||
==Sign out== | |||
===Suggestive FNA=== | |||
<pre> | |||
Lymph Node, Right Neck, FNA: | |||
- Large binucleated and multinucleated cells with macronucleoli in | |||
a background of abundant lymphocytes, histiocytes, rare eosinophils. | |||
Comment: | |||
A cell block is not available for further work-up. The findings raise the possibility of Hodgkin's lymphoma. | |||
A further biopsy is required for the diagnosis. | |||
</pre> | |||
==See also== | ==See also== | ||
Latest revision as of 22:01, 4 December 2018
| Classical Hodgkin lymphoma | |
|---|---|
| Diagnosis in short | |
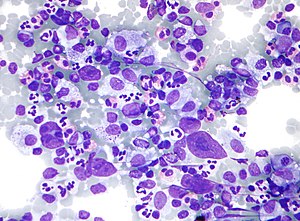 HL mixed cellularity - cytology. | |
|
| |
| LM | Reed-Sternberg cell (large binucleated cell (>= 45 micrometres), +/-multinucleated, +/-horseshoe-like shape, macronucleolus - approximately the size of a RBC (~8 micrometers)), well-defined cell border, abundant cytoplasm. |
| Subtypes | nodular sclerosis CHL, mixed cellularity CHL, lymphocyte-rich CHL, lymphocyte-depleted CHL |
| LM DDx |
diffuse large B cell lymphoma (esp. T-cell/histiocytic-rich LBCL), anaplastic large cell lymphoma, B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma, nodular lymphocyte-predominant Hodgkin lymphoma |
| IHC | CD30 Reed-Sternberg cells (RSCs) +ve ~98%, CD15 Reed-Sternberg cells +ve ~80% (also stains neutrophils), CD45 often negative in RSCs, CD20 -ve/+ve, PAX5 +ve |
| Site | usu. lymph node - classically in the neck |
|
| |
| Clinical history | young adults, older adults (bimodal distribution) |
| Signs | lymphadenopathy - usu. neck, +/-B symptoms (fever, night sweats, weight loss) |
| Prevalence | common |
| Prognosis | usu. good, dependent on stage |
Hodgkin lymphoma, abbreviated HL, is a haematological malignancy. If not otherwise specified, Hodgkin lymphoma generally refers to classical Hodgkin lymphoma (CHL) rather than nodular lymphocyte-predominant Hodgkin lymphoma (NLPHL). The latter accounts for only about 5% of the loose label of Hodgkin lymphoma[1] and shows a sufficiently different biology and immunophenotype that is essentially a different disease (see main article on NLPHL). The common feature is large atypical cells: Hodgkin/Reed-Sternberg cells in the case of classical Hodgkin lymphoma and "popcorn"/lymphohistiocytic/L&H cells in NLPHL. However, at least in typical cases, there are morphological and immunophenotypic differences.
Classical Hodgkin lymphoma has a bi-modal distribution, afflicting young adults and with a further peak in incidence in middle-age. Fortunately, it usually has a good prognosis.
Pathologists say "... it is both the easiest and hardest diagnosis to make." The reason for this is: the diagnosis depends on finding Reed-Sternberg cells (or Popcorn cells); if they are obvious the diagnosis is easy... if you can't find 'em and an alternative diagnosis is not apparent -- you wonder whether you're missing them.
General
Clinical
Symptoms:[1]
- "B symptoms" - all required:[2] weight loss, night sweats and fever.
- Infections due to immune dysfunction.
Diagnosis:
- HL cannot be diagnosed with standard flow cytometry (FC) - but has been diagnosed with specialized FC.[3]
Prognosis:
- Usually good.
- Unlike non-Hodgkin lymphomas, it spreads in a predictable pattern; thus, staging plays an important role in determining the therapy.[4]
- Clinically classified into early favourable, early unfavourable and late/advanced disease.
Classic HL sub-types
Subtypes of classic HL
There are four CHL subtypes:[1]
- Nodular sclerosis CHL - ~70% of CHL.
- Mixed cellular background - T cell, plasma cells, eosinophils, neutrophils and histiocytes.
- Nodular sclerosing fibrosis - thick strands fibrosis.
- Mixed cellularity CHL - ~20-25% of CHL.
- Lymphocyte-rich CHL - rare.
- T lymphocytes only (no mix of cells).
- Lymphocyte-depleted CHL - rare.
- May be associated with HIV infection.[5]
Memory device:
- The subtypes prevalence is in reverse alphabetical order.
Gross
Location:
- Almost always arises from a lymph node - classically in the neck, but may be in the axilla and mediastinum
- Spleen may be involved
- Bone marrow involvement is unusual (~5% of cases, higher in HIV-associated cases), so bone marrow assessment is usually not performed
- Extranodal Hodgkin lymphoma is (case report) rare.[6]
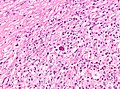
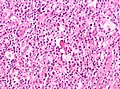
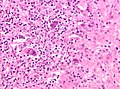
Microscopic
Defined by Reed-Sternberg cells (RSCs). Morphologically similar mononuclear cells are known as Hodgkin cells. RSCs are:
- Large binucleated cell (>= 45 micrometres).[7]
- May be multinucleated.
- May have a horseshoe-like shape.
- Macronucleolus - approximately the size of a RBC (~8 micrometers).
- Well-defined cell border.
- Abundant cytoplasm.
RSC may show peri-cellular clearing, making the cells appear within a space. These are called lacunar cells (as they are in a "lake"). Apoptotic RSC may show pyknotic nuclei and scant eosinophilic cytoplasm and are sometimes known as "mummified" cells.
Images (classic HL)
DDx both CHL & NLPHL
- CHL/NLPHL.
- Diffuse large B cell lymphoma (DLBCL), esp. T-cell/histiocytic-rich LBCL.
- Anaplastic large cell lymphoma (ALCL).
- B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma.[8] (typically in cases of numerous large atypical cells where the morphology and immunophenotype do not neatly fit into either DLBCL or CHL).
IHC
Abbreviated panel:[9]
- CD30 Reed-Sternberg cells (RSCs) +ve ~98% (beware of mis-interpreting CD30+ activated lymphoid cells)
- CD15 Reed-Sternberg cells +ve ~80%, stains neutrophils.
- Both CD30 and CD15 are classically positive in a membranous and Golgi pattern
- MUM1 +ve
- CD45 often negative in RSCs.
- CD20 may stain RSCs (usually negative, but can be weak).
- PAX5 +ve, though said to be weaker than background normal B-cells[10]
Additional - for completeness:
- CD3 (T lymphocytes) - negative in RSCs
- OCT2/BOB1 negative (co-transcription factors for immunoglobulin production, one or the other is usually negative)
- 40% are EBV positive.
NLPHL IHC differs from the classical HL:[10]
- LCA +ve.
- CD20 +ve.
- CD10 +ve.
- Bcl-6 +ve.
- EMA +ve (40-50%)
- CD30 -ve
- CD15 -ve.
A panel
| Antibody | NLPHL | CHL |
| CD45 | +ve | -ve |
| CD20 | +ve | -ve |
| BCL6 | +ve | -ve |
| MUM1[11] | -ve | +ve |
| CD30 | -ve | +ve (most sensitive). |
| CD15 | -ve | +ve |
| CD21 | networks present | no networks |
| CD23 | networks present | no networks |
| OCT-2 | +ve | -ve |
| PAX5 | +ve | +ve (proves B cell linage) |
| CD3 | usu. < benign B cell | usu. > benign B cell component |
| CD57 | rosettes around malign. cells | - |
| EBER | -ve | +ve/-ve |
| EMA | +ve/-ve | -ve |
| 4 unstained |
Sign out
Suggestive FNA
Lymph Node, Right Neck, FNA: - Large binucleated and multinucleated cells with macronucleoli in a background of abundant lymphocytes, histiocytes, rare eosinophils. Comment: A cell block is not available for further work-up. The findings raise the possibility of Hodgkin's lymphoma. A further biopsy is required for the diagnosis.
See also
References
- ↑ 1.0 1.1 1.2 Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 567. ISBN 978-0781765275.
- ↑ URL: http://lymphoma.about.com/od/symptoms/f/bsymptoms.htm. Accessed on: 11 August 2010.
- ↑ Fromm JR, Thomas A, Wood BL (March 2009). "Flow cytometry can diagnose classical hodgkin lymphoma in lymph nodes with high sensitivity and specificity". Am. J. Clin. Pathol. 131 (3): 322–32. doi:10.1309/AJCPW3UN9DYLDSPB. PMID 19228638.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 315. ISBN 978-1416054542.
- ↑ 5.0 5.1 Sissolak G, Sissolak D, Jacobs P (April 2010). "Human immunodeficiency and Hodgkin lymphoma". Transfus. Apher. Sci. 42 (2): 131–9. doi:10.1016/j.transci.2010.01.008. PMID 20138008.
- ↑ Vadmal, MS.; LaValle, GP.; DeYoung, BR.; Frankel, WL.; Marsh, WL. (Dec 2000). "Primary localized extranodal hodgkin disease of the transverse colon.". Arch Pathol Lab Med 124 (12): 1824-7. doi:10.1043/0003-9985(2000)1241824:PLEHDO2.0.CO;2. PMID 11100066.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 329. ISBN 978-1416054542.
- ↑ Gualco, G.; Natkunam, Y.; Bacchi, CE. (Jan 2012). "The spectrum of B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma: a description of 10 cases.". Mod Pathol. doi:10.1038/modpathol.2011.200. PMID 22222636.
- ↑ Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 568. ISBN 978-0781765275.
- ↑ 10.0 10.1 Lefkowitch, Jay H. (2006). Anatomic Pathology Board Review (1st ed.). Saunders. pp. 683. ISBN 978-1416025887.
- ↑ URL: http://www.ncbi.nlm.nih.gov/omim/601900. Accessed on: 10 August 2010.