Difference between revisions of "Metaphyseal fibrous defect"
Jump to navigation
Jump to search
| (7 intermediate revisions by one other user not shown) | |||
| Line 7: | Line 7: | ||
| Micro = | | Micro = | ||
| Subtypes = | | Subtypes = | ||
| LMDDx = [[giant cell tumour of bone]] | | LMDDx = [[giant cell tumour of bone]], others | ||
| Stains = | | Stains = | ||
| IHC = | | IHC = | ||
| Line 29: | Line 29: | ||
| ClinDDx = | | ClinDDx = | ||
| Tx = none | | Tx = none | ||
}} | |||
{{ Infobox external links | |||
| Name = {{PAGENAME}} | |||
| EHVSC = | |||
| EHVSC_mult = | |||
| pathprotocols = | |||
| wikipedia = Nonossifying fibroma | |||
| pathoutlines = {{Pathologyoutlines|topic/bonemetaphysealfibrousdefect}} | |||
| rosaicollection = | |||
}} | }} | ||
'''Metaphyseal fibrous defect''', abbreviated '''MFD''', is a common benign abnormality of the [[metaphysis]], classically seen in children and young adults. | '''Metaphyseal fibrous defect''', abbreviated '''MFD''', is a common benign abnormality of the [[metaphysis]], classically seen in children and young adults. | ||
| Line 41: | Line 50: | ||
*Often small lesions discovered as an radiographic incidentaloma. | *Often small lesions discovered as an radiographic incidentaloma. | ||
*Rarely seen as a pathologic specimen (should not be biopsied). | *Rarely seen as a pathologic specimen (should not be biopsied). | ||
*May be seen in the context of ''Jaffe-Campanacci syndrome''.<ref>URL: [http://www.bonetumor.org/plasma-cell-tumors/jaffe-campanacci-syndrome http://www.bonetumor.org/plasma-cell-tumors/jaffe-campanacci-syndrome]. Accessed on: October 14, 2014.</ref> | *May be seen in the context of ''Jaffe-Campanacci syndrome'' which may be a presentation of Neurofibromatosis Type 1.<ref>URL: [http://www.bonetumor.org/plasma-cell-tumors/jaffe-campanacci-syndrome http://www.bonetumor.org/plasma-cell-tumors/jaffe-campanacci-syndrome]. Accessed on: October 14, 2014.</ref><ref>{{Cite journal | last1 = Stewart | first1 = DR. | last2 = Brems | first2 = H. | last3 = Gomes | first3 = AG. | last4 = Ruppert | first4 = SL. | last5 = Callens | first5 = T. | last6 = Williams | first6 = J. | last7 = Claes | first7 = K. | last8 = Bober | first8 = MB. | last9 = Hachen | first9 = R. | title = Jaffe-Campanacci syndrome, revisited: detailed clinical and molecular analyses determine whether patients have neurofibromatosis type 1, coincidental manifestations, or a distinct disorder. | journal = Genet Med | volume = 16 | issue = 6 | pages = 448-59 | month = Jun | year = 2014 | doi = 10.1038/gim.2013.163 | PMID = 24232412 }} | ||
</ref> | |||
*Radiographic diagnosis. | |||
Clinical history: | Clinical history: | ||
| Line 47: | Line 58: | ||
*Pathologic fracture. | *Pathologic fracture. | ||
Treatment: | |||
* | *None (spontaneously resolve by ossification). | ||
* | **Diagnosis is part of the ''skeletal do not touch list''.<ref>URL: [http://radiopaedia.org/articles/skeletal-do-not-touch-lesions-1 http://radiopaedia.org/articles/skeletal-do-not-touch-lesions-1]. Accessed on: October 14, 2014.</ref> | ||
Notes: | |||
*May resolve into a 'bone island'. | *May resolve into a ''bone island''. | ||
Clinical DDx: | |||
*''FOG MACHINES'' acronym for radiographically lytic bone lesions.<ref>URL: [http://radiopaedia.org/articles/lytic-bone-lesion-mnemonic http://radiopaedia.org/articles/lytic-bone-lesion-mnemonic]. Accessed on: October 14, 2014.</ref> | |||
==Gross== | |||
*Firm, granular, brown to yellow to red. | |||
Site: | |||
*Metaphysis of distal femur or proximal tibia (80%). | *[[Metaphysis]] of distal femur or proximal tibia (80%). | ||
*Cortical. | *Cortical. | ||
* | *Metaphysis. | ||
*Long bones. | *Long bones. | ||
*Eccentric location. | *Eccentric location. | ||
== | ===Radiology=== | ||
* | *Sharply demarcated, lucent, loculated, meta-diaphyseal lesion. | ||
*Surrounded by a rim of sclerotic bone. | |||
<gallery> | |||
Image:NOF 1.jpg|Nonossifying fibroma. (WC) | |||
</gallery> | |||
==Microscopic== | ==Microscopic== | ||
| Line 73: | Line 95: | ||
DDx (microscopic): | DDx (microscopic): | ||
*[[Giant cell tumour of bone]] - [[epiphysis|epiphyseal]] location, occurs in adults. | *[[Giant cell tumour of bone]] - [[epiphysis|epiphyseal]] location, occurs in adults. | ||
*Other [[giant cell lesions]] of bone. | |||
*[[Spindle cell lesion]]s of bone. | |||
* | |||
==Images== | ==Images== | ||
| Line 97: | Line 113: | ||
==IHC== | ==IHC== | ||
*Not relevant | *Not relevant. | ||
==Molecular== | ==Molecular== | ||
*Not relevant | *Not relevant. | ||
==Sign out== | ==Sign out== | ||
<pre> | <pre> | ||
BONE, CURETTAGE: METAPHYSEAL FIBROUS DEFECT / NONOSSIFYING FIBROMA. | BONE, CURETTAGE: | ||
- METAPHYSEAL FIBROUS DEFECT / NONOSSIFYING FIBROMA. | |||
</pre> | </pre> | ||
| Line 117: | Line 131: | ||
==External links== | ==External links== | ||
*http://njms2.umdnj.edu/tutorweb/case8.htm | *[http://njms2.umdnj.edu/tutorweb/case8.htm A case of MFD (umdnj.edu)]. | ||
*[http://radiopaedia.org/articles/fibrous-cortical-defect Fibrous cortical defect (radiopaedia.org)]. | |||
*http://radiopaedia.org/articles/fibrous-cortical-defect | *[http://radiopaedia.org/articles/non-ossifying-fibroma-1 Non-ossifying fibroma (radiopaedia.org)]. | ||
*http://radiopaedia.org/articles/non-ossifying-fibroma-1 | |||
[[Category:Diagnosis]] | [[Category:Diagnosis]] | ||
[[Category:Bone]] | |||
Latest revision as of 23:43, 18 October 2014
Metaphyseal fibrous defect, abbreviated MFD, is a common benign abnormality of the metaphysis, classically seen in children and young adults.
| Metaphyseal fibrous defect | |
|---|---|
| Diagnosis in short | |
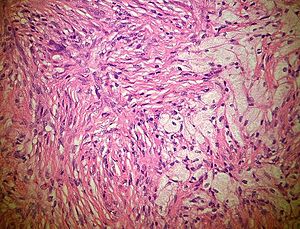 | |
|
| |
| Synonyms | nonossifying fibroma, fibrous cortical defect, fibrous metaphyseal defect, fibroxanthoma of bone |
| LM DDx | giant cell tumour of bone, others |
| Site | metaphysis of bone - usu. lower extremity |
|
| |
| Clinical history | incidental radiograhic finding |
| Prevalence | common |
| Radiology | lucent defect |
| Prognosis | benign |
| Treatment | none |
| Metaphyseal fibrous defect | |
|---|---|
| External resources | |
| Wikipedia | Nonossifying fibroma |
| Pathology Outlines | topic/bonemetaphysealfibrousdefect |
They are also known as fibrous cortical defect, fibrous metaphyseal defect, and fibroxanthoma of bone. Nonossifying fibroma is a larger lesion but otherwise identical.
General
- Common.
- Non-neoplastic.
- Self-limited.
- Skeletally immature individuals, children and adolescents.
- Often small lesions discovered as an radiographic incidentaloma.
- Rarely seen as a pathologic specimen (should not be biopsied).
- May be seen in the context of Jaffe-Campanacci syndrome which may be a presentation of Neurofibromatosis Type 1.[1][2]
- Radiographic diagnosis.
Clinical history:
- Incidental radiographic finding.
- Pathologic fracture.
Treatment:
- None (spontaneously resolve by ossification).
- Diagnosis is part of the skeletal do not touch list.[3]
Notes:
- May resolve into a bone island.
Clinical DDx:
- FOG MACHINES acronym for radiographically lytic bone lesions.[4]
Gross
- Firm, granular, brown to yellow to red.
Site:
- Metaphysis of distal femur or proximal tibia (80%).
- Cortical.
- Metaphysis.
- Long bones.
- Eccentric location.
Radiology
- Sharply demarcated, lucent, loculated, meta-diaphyseal lesion.
- Surrounded by a rim of sclerotic bone.
Microscopic
Features:
- Spindle cells without cytologic atypia are arranged in a storiform pattern.
- Scattered chronic inflammatory cells and benign giant cells.
- Foam cells and hemosiderin deposition are present.
- Mitoses are seen but cytologic atypia is absent.
DDx (microscopic):
- Giant cell tumour of bone - epiphyseal location, occurs in adults.
- Other giant cell lesions of bone.
- Spindle cell lesions of bone.
Images
www:
Stains
- Not relevant.
IHC
- Not relevant.
Molecular
- Not relevant.
Sign out
BONE, CURETTAGE: - METAPHYSEAL FIBROUS DEFECT / NONOSSIFYING FIBROMA.
See also
- Bone.
References
- ↑ URL: http://www.bonetumor.org/plasma-cell-tumors/jaffe-campanacci-syndrome. Accessed on: October 14, 2014.
- ↑ Stewart, DR.; Brems, H.; Gomes, AG.; Ruppert, SL.; Callens, T.; Williams, J.; Claes, K.; Bober, MB. et al. (Jun 2014). "Jaffe-Campanacci syndrome, revisited: detailed clinical and molecular analyses determine whether patients have neurofibromatosis type 1, coincidental manifestations, or a distinct disorder.". Genet Med 16 (6): 448-59. doi:10.1038/gim.2013.163. PMID 24232412.
- ↑ URL: http://radiopaedia.org/articles/skeletal-do-not-touch-lesions-1. Accessed on: October 14, 2014.
- ↑ URL: http://radiopaedia.org/articles/lytic-bone-lesion-mnemonic. Accessed on: October 14, 2014.