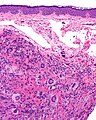
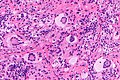
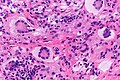
Juvenile xanthogranuloma
Jump to navigation
Jump to search
The printable version is no longer supported and may have rendering errors. Please update your browser bookmarks and please use the default browser print function instead.
| Juvenile xanthogranuloma | |
|---|---|
| Diagnosis in short | |
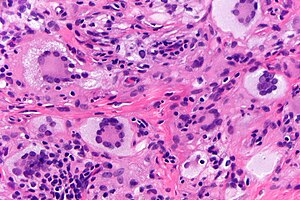 Juvenile xanthogranuloma. H&E stain. | |
|
| |
| LM | dermal histiocytes with abundant cytoplasm, +/-Touton giant cells (large multi-nucleated cells where nuclei are distributed at the cell periphery) |
| LM DDx | Langerhans cell histiocytosis, Spitz nevus (reported to have Touton cells), Dermatofibroma - aneurysmal type |
| IHC | CD68 +ve, CD1a -ve, CD207 -ve |
| Site | skin |
|
| |
| Clinical history | usually in children and infants, sometimes in adults |
| Prognosis | benign |
Juvenile xanthogranuloma, abbreviated JXG, is a relatively common distinctive diagnosis in dermatopathology. It is also known as nevoxanthoendothelioma. In adults, it is called adult xanthogranuloma.[1]
General
- Usually in children and infants, sometimes in adults.[1]
- Most common form of non–Langerhans cell histiocytosis.[4]
- Can rarely be found in the brain.[5]
Microscopic
Features:[4]
- Dermal histiocytes:
- Abundant cytoplasm - may not be xanthomatous/foam cells.
- +/-Touton giant cell - key feature.
- Large multi-nucleated cells where nuclei are distributed at the cell periphery.
Notes:
- Must prove they are non-Langerhans cell histiocytes, esp. if no Touton giant cells.
DDx:
- Langerhans cell histiocytosis.
- Spitz nevus - uncommon; reported to have Touton cells.[6]
- Dermatofibroma, aneurysmal - has Touton giant cells and hemosiderin deposition.
- Tuberculoma.
- Erdheim-Chester disease - usu. BRAF V600E mutated.[7]
- Rosai-Dorfman disease - Emperipolesis.
- Necrobiotic xanthogranuloma - also may have Touton giant cells.
Images
IHC
Features:[4]
- Langerhans cell markers: CD1a, CD207 -- both should be negative.
- If Touton giant cells are absent -- this is essential.
- Histiocyte markers: CD68, CD163 -- both should be positive.
- Vimentin +ve.
Other markers:[8]
- CD4 +ve (21 of 27 cases).
- CD45 +ve (25 of 27 cases).
- Factor XIIIa +ve (25 of 27 cases).
Negatives:[9]
- Muscle markers: actin, desmin.
- Others: S100, factor VIII, cytokeratins.
Sign out
SKIN LESION, CHIN, BIOPSY: - JUVENILE XANTHOGRANULOMA.
See also
References
- ↑ 1.0 1.1 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 622. ISBN 978-0443066542.
- ↑ Chiang, E.; Lissner, G.; Bryar, PJ.. "Unusual presentation of xanthogranuloma on the eyelid of an adult.". Ophthal Plast Reconstr Surg 30 (6): e155-6. doi:10.1097/01.iop.0000440703.67932.37. PMID 24801255.
- ↑ Tan, LC.; Tan, KB.; Aw, CW. (Feb 2014). "Unusual presentation of adult xanthogranuloma: a case report.". Singapore Med J 55 (2): e25-7. doi:10.11622/smedj.2013207. PMID 24154556.
- ↑ 4.0 4.1 4.2 URL: http://emedicine.medscape.com/article/1111629-diagnosis. Accessed on: 3 February 2011.
- ↑ URL: http://path.upmc.edu/cases/case245/dx.html. Accessed on: 13 January 2012.
- ↑ Guitart, J.; Gerami, P. (Jul 2008). "Touton-like giant cells in a Spitz's nevus.". J Cutan Pathol 35 (7): 694-5. doi:10.1111/j.1600-0560.2007.00877.x. PMID 18312437.
- ↑ Haroche, J.; Charlotte, F.; Arnaud, L.; von Deimling, A.; Hélias-Rodzewicz, Z.; Hervier, B.; Cohen-Aubart, F.; Launay, D. et al. (Sep 2012). "High prevalence of BRAF V600E mutations in Erdheim-Chester disease but not in other non-Langerhans cell histiocytoses.". Blood 120 (13): 2700-3. doi:10.1182/blood-2012-05-430140. PMID 22879539.
- ↑ Kraus, MD.; Haley, JC.; Ruiz, R.; Essary, L.; Moran, CA.; Fletcher, CD. (Apr 2001). "Juvenile xanthogranuloma: an immunophenotypic study with a reappraisal of histogenesis.". Am J Dermatopathol 23 (2): 104-11. PMID 11285404.
- ↑ Thomas DB, Sidler AK, Huston BM (October 1998). "Radiological case of the month. Juvenile xanthogranuloma". Arch Pediatr Adolesc Med 152 (10): 1029–30. PMID 9790615. http://archpedi.ama-assn.org/cgi/content/full/152/10/1029.