Difference between revisions of "Diffuse alveolar damage"
Jump to navigation
Jump to search
(touch) |
|||
| Line 2: | Line 2: | ||
{{ Infobox diagnosis | {{ Infobox diagnosis | ||
| Name = {{PAGENAME}} | | Name = {{PAGENAME}} | ||
| Image = Hyaline membranes - very high mag.jpg | | Image = Hyaline membranes - very high mag.jpg | ||
| Width = | | Width = | ||
| Caption = Hyaline membranes. [[H&E stain]]. | | Caption = Hyaline membranes. [[H&E stain]]. | ||
Revision as of 03:26, 30 June 2015
| Diffuse alveolar damage | |
|---|---|
| Diagnosis in short | |
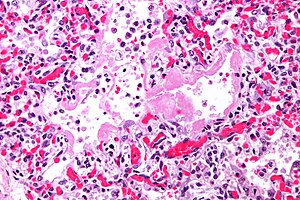 Hyaline membranes. H&E stain. | |
|
| |
| LM | dependent on phase - exudative: hyaline membranes; proliferative: interstitial thickening, inflammation (lymphocytes), type 2 pneumocyte hyperplasia, edema, Masson bodies in the airway, hyaline material (usu. focal); fibrotic: interstitial inflammation, interstitial fibrosis |
| Subtypes | exudative, proliferative, fibrotic |
| LM DDx | organizing pneumonia (especially for proliferative phase DAD), bronchiolitis obliterans |
| Site | lung - see diffuse lung diseases |
|
| |
| Prognosis | often poor, dependent on severity and comorbidities |
| Other | histologic correlate of: acute respiratory distress syndrome (ARDS), acute interstitial pneumonia (AIP), transfusion related acute lung injury (TRALI) |
| Treatment | dependent on underlying cause |
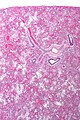
Diffuse alveolar damage, abbreviated DAD, is a relatively common lung pathology that is grouped with the diffuse lung diseases and has several clinical correlates.
General
Etiology:
- Abrupt hypoxemia with pulmonary infiltrates leading to epithelial cell and endothelial cell death not accompanied by cardiac failure.[1]
DAD is the histologic correlate of:
- Acute respiratory distress syndrome (ARDS).
- AKA adult respiratory distress syndrome (ARDS) to differentiate it from respiratory distress syndrome in infants.
- Acute interstitial pneumonia (AIP).
- Transfusion related acute lung injury (TRALI).
The DDx is broad:[2]
- Infection/sepsis.
- Toxic (smoke, oxygen).
- Drug (amiodarone, chemotherapy).
- Trauma/shock.
- Inflammatory.
- Idiopathic.
Microscopic
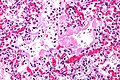
- Exudative:
- Hyaline membranes - key feature.
- Debris (pink crap) lines the alveolar spaces.
- Hyaline membranes - key feature.
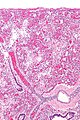
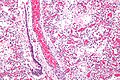
- Proliferative:
- Interstitial thickening.
- Inflammation (lymphocytes).
- Hobnailing of alveolar lining cells (type 2 pneumocyte hyperplasia[5]).
- Edema (link pink crap in the alveoli).
- Masson bodies in the airway.
- Hyaline material (usu. focal) - key feature.
- Fibrotic:
- Interstitial inflammation.
- Fibrosis.
DDx:[4]
- Cryptogenic organizing pneumonia - especially for proliferative phase DAD.
- Bronchiolitis obliterans.
Images
www:
- Proliferative phase DAD - intermed. mag. (flickr.com/Yale Rosen).
- Proliferative phase DAD - high mag. (flickr.com/Yale Rosen).
See also
References
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 364. ISBN 978-1416054542.
- ↑ Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 91. ISBN 978-0781765275.
- ↑ Klatt, Edward C. (2006). Robbins and Cotran Atlas of Pathology (1st ed.). Saunders. pp. 103. ISBN 978-1416002741.
- ↑ 4.0 4.1 Castro, CY. (2006). "ARDS and diffuse alveolar damage: a pathologist's perspective.". Semin Thorac Cardiovasc Surg 18 (1): 13-9. doi:10.1053/j.semtcvs.2006.02.001. PMID 16766248.
- ↑ URL: http://d3jonline.tripod.com/20-Pulmonary_II/Pathology_of_Interstitial_Lung_Diseases.htm. Accessed on: 22 February 2012.