Thrombotic microangiopathy
Jump to navigation
Jump to search
The printable version is no longer supported and may have rendering errors. Please update your browser bookmarks and please use the default browser print function instead.
| Thrombotic microangiopathy | |
|---|---|
| Diagnosis in short | |
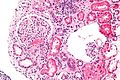
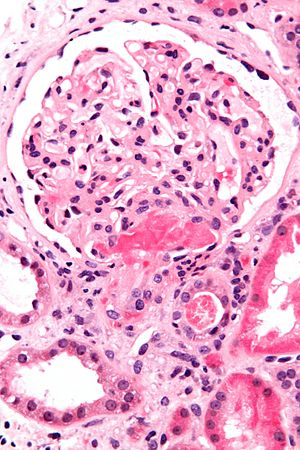 Acute thrombotic microangiopathy. H&E stain. | |
|
| |
| LM | microvascular occlusion with "loose" intimal thickening - fluffy appearing intima, fibrin entrapped RBCs, +/-onion skin-like appearance (chronic change) |
| Subtypes | acute, chronic |
| LM DDx | vasculitis, small vessel |
| Site | blood vessels - esp. kidney |
|
| |
| Clin. DDx | DDx for TMA: malignant hypertension, DIC, APLA in SLE, scleroderma renal crisis, HIV associated TTP, reaction to chemotherapy, calcineurin inhibitor toxicity |
| Treatment | dependent on underlying cause |
Thrombotic microangiopathy, abbreviated TMA, is a group of disorders affecting small blood vessels. Microangiopathic is a disease affecting small blood vessels.[1]
Differential diagnosis
Clinical
Others:[4]
- Malignant hypertension.[5]
- DIC.
- APLA[6] in SLE.
- Scleroderma renal crisis.
- HIV associated TTP.
- Chemotherapy.
- Calcineurin inhibitor toxicity.
Notes:
- The above cannot be differentiated on a histomorphologic basis.
Histologic
The histomorphologic differential diagnosis is:
- Vasculitis.
- Inflammatory cells within the vessel wall.
- Vessel wall injury, i.e. necrosis.
General
- Underlying pathology: endothelial cell damage.
Microscopic
Features:[7]
- Microvascular occlusion.[8]
- "Loose" intimal thickening; fluffy appearing intima.
- May be have an onion skin-like appearance.
- Fibrin entrapped RBCs.
Notes:
- The last two (#2 and #3) are useful for discrimination from endarteritis.[7]
- Early finding: endothelial cell swelling.
Images
www:
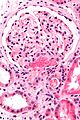
Acute changes:
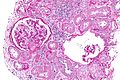
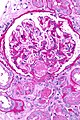
Chronic changes:
See also
References
- ↑ URL: http://www.mercksource.com/pp/us/cns/cns_hl_dorlands_split.jsp?pg=/ppdocs/us/common/dorlands/dorland/one/000005089.htm. Accessed on: 9 September 2010.
- ↑ URL: http://emedicine.medscape.com/article/779218-overview. Accessed on: 8 November 2010.
- ↑ Mayer SA, Aledort LM (May 2005). "Thrombotic microangiopathy: differential diagnosis, pathophysiology and therapeutic strategies". Mt. Sinai J. Med. 72 (3): 166–75. PMID 15915311.
- ↑ Benz, K.; Amann, K. (May 2010). "Thrombotic microangiopathy: new insights.". Curr Opin Nephrol Hypertens 19 (3): 242-7. doi:10.1097/MNH.0b013e3283378f25. PMID 20186056.
- ↑ Zhang, B.; Xing, C.; Yu, X.; Sun, B.; Zhao, X.; Qian, J. (Mar 2008). "Renal thrombotic microangiopathies induced by severe hypertension.". Hypertens Res 31 (3): 479-83. doi:10.1291/hypres.31.479. PMID 18497467.
- ↑ Asherson, RA. (1998). "The catastrophic antiphospholipid syndrome, 1998. A review of the clinical features, possible pathogenesis and treatment.". Lupus 7 Suppl 2: S55-62. PMID 9814675.
- ↑ 7.0 7.1 Fogo, Agnes; Bruijn, Jan A.; Cohen, Arthur H.; Colvin, Robert B.;Jennette, J. Charles (2006). Fundamentals of Renal Pathology (1st ed.). Springer. pp. 204. ISBN 978-0387311265.
- ↑ Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 670. ISBN 978-1416031215.
- ↑ Ruggenenti, P.; Noris, M.; Remuzzi, G. (Sep 2001). "Thrombotic microangiopathy, hemolytic uremic syndrome, and thrombotic thrombocytopenic purpura.". Kidney Int 60 (3): 831-46. doi:10.1046/j.1523-1755.2001.060003831.x. PMID 11532079.