Non-malignant skin disease
Non-malignant skin disease is relatively common. The pathology may or may not be specific. Some diseases require clinical information to diagnose.
An introduction to dermatopathology is in the dermatopathology article. Nevi (moles) and other melanocytic lesions are dealt with in the article melanocytic lesions. Inflammatory skin conditions are dealt with in inflammatory skin disorders.
Other
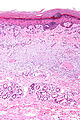
Lichen simplex chronicus
Prurigo nodularis
General
- Can be thought of as a localized/focal version of lichen simplex chronicus (LSC).
Gross
- Dome-shaped/raised - papular (<1 cm) or nodular (>1 cm).[2]
Microscopic
DDx:
- Lichen simplex chronicus - a more diffuse process, not a raised lesion.
Sign out
SKIN LESION, LEFT CHIN, BIOPSY: - PRURIGO NODULARIS.
Micro
The sections show a raised lesion with compact hyperkeratosis and irregular acanthosis. Spongiosis is seen focally. There is minimal hypergranulosis.
There is no thinning of the suprapapillary plate and no dilated superficial blood vessels. There is no interface activity.
Very common
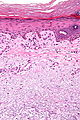
Dermatomycosis
- Dermatophytosis redirects here.
General
- Fungal infection of skin.
Note:
- Dermatophytosis (ring worm) is a type of dermatomycosis.
Microscopic
Features:
- Microorganisms - key feature.
- Often hyphae (candida) - like twigs of a tree... branching.
- May be very fragmented in section ~ size of a neutrophil.
- Often hyphae (candida) - like twigs of a tree... branching.
- Perivascular inflammation, esp. neutrophils.
- Exocytosis - blood cell infiltrate the epidermis.
Images:
- WC:
- www:
Stains
Sign out
SKIN, BIOPSY: - SKIN WITH SUPERFICIAL FUNGAL ORGANISMS CONSISTENT WITH CANDIDA. - REACTIVE CHANGES OF THE EPITHELIUM.
Micro
The sections show skin with a neutrophilic infiltrate in the superficial epidermis. PAS-D staining demonstrates fungal organisms with a morphology suggestive of candida.
The epithelium has parakeratosis, acanthosis and spongiosis. No mitotic activity is appreciated. The keratinocytes are moderately enlarged and have evident nucleoli.
Cicatrix
Fibroepithelial polyp
General
- Benign.
- Older people.
- May be associated with pregnancy, diabetes, intestinal polyposis.[4]
- Can be a component of Birt–Hogg–Dubé syndrome.
Gross
- Raised skin-coloured lesion.
Image:
Microscopic
Features:
- On a stalk / epithelium on three sides.
- Benign epidermis.
DDx:
- Pedunculated seborrheic keratosis - typically have epidermal hyperplasia, hyperkeratosis, horn cysts.[5]
- Regressing melanocytic lesions.
- Nevus lipomatosus superficialis - abundant adipocytes in the superficial dermis.
- Neurofibroma.
Images:
- Fibroepithelial polyp (dermatlas.med.jhmi.edu).[6]
- Fibroepithelial polyp (surgicalpathologyatlas.com).
- Inflamed fibroepithelial polyp (cdlib.org).[7]
Sign out
EYELID ("TAG"), RIGHT, REMOVAL:
- BENIGN FIBROEPITHELIAL POLYP.
SKIN ("SKIN TAG"), THIGH, REMOVAL:
- FIBROEPITHELIAL POLYP.
Micro
The sections show a fragment of skin with epithelium on three sides. The epithelium matures normally and is not hypertrophic. Orthokeratosis is present. The core of the lesion has fibrous tissue. There is no significant inflammation. No melanocytic nests are identified.
Inflamed
The sections show a fragment of skin with epithelium on three sides. The epithelium matures and is acanthotic. Minimal parakeratosis is present. The core of the lesion consists of fibrous tissue with a mild lymphocyte-predominant dermal infiltrate. Rare siderophages are present.
There is mild basal nuclear enlargement. No significant nuclear atypia is apparent. The dermal-epidermal interface is well-demarcated. Rare basal mitotic activity is identified.
Actinic keratosis
Actinic cheilitis
General
- Actinic keratosis of the lip.[8]
Microscopic
- See actinic keratosis.
Sign out
LESION, LOWER LIP, BIOPSY: - ACTINIC CHEILITIS. - SOLAR ELASTOSIS.
Micro
The sections show skin with moderate basal nuclear hyperchromasia and atypia, and parakeratosis. The squamous epithelium has maturation to the surface. There is no inflammation at the dermal-epidermal interface. Solar elastosis is present.
Seborrheic keratosis
Pilomatricoma
Dermatofibroma
Ezcema
General
- A nebulous thingy.
- Very common.
DDx:
- Contact allergy.
- Drug reaction.
- Food allergy.
Microscopic
Features:[9]
- Spongiosis (epidermal edema); keratinocytes spacing increased - key feature.
- +/-Interdermal vesicles.
- +/-Eosinophils (may suggest Rx reaction).
- Perivascular lymphocytes.
Acne vulgaris
General
- Extremely common - esp. among adolescents.
- Very rarely seen by pathologists.
Treatments:
- Antibiotic (minocycline).
- Isotretinoin AKA all-trans retinoic acid (ATRA).
Gross
- Papules, pustules, nodules or cysts.
- White, black or erythematous.
Images:
Microscopic
Features:[10]
- Folliculitis:[11]
- Neutrophils around hair follicle and infiltrate into it - including the follicular canal.
- Epidermal invagination or cyst at site of a hair follicle - contains:
- Sebum.
- +/-Bacteria (Propionibacterium acnes) and inflammatory cells - typically neurophils.
Subtyped into:
- Open comedones ("blackheads") - no extension to epidermal surface.
- Closed comedones ("whiteheads") - to epidermal surface have wide opening.
DDx - acneiform disorder:[11]
- Rosacea.
- Infective folliculitis.
- Perioral dermatitis.
- Acne vulgaris.
Image:
Solar elastosis
General
- Very common.
- Caused by sun exposure - specifically UV light.[13]
- Severity correlated with cumulative exposure to UV light..[14]
- Often co-localized with skin cancers - as UV light is risk factor for skin cancers.[14]
- Benign.
Microscopic
Features:
- Grey, spaghetti-like material in the superficial dermis.
DDx:
Note:
- The DDx above is things associated with sun damaged skin.
- Dermal mucin (as my be seen in lupus erythematosus) is a possible mimic - but it isn't spaghetti-like and the "background" (an interface dermatitis) is different.
Images
www:
Sign out
SKIN, RIGHT CHEEK, RE-EXCISION: - DERMAL SCAR. - EXTENSIVE SOLAR ELASTOSIS.
Prominent blood vessels
SKIN LESION, LEFT CHEEK, BIOPSY: - SKIN WITH SOLAR ELASTOSIS AND PROMINENT SMALL BLOOD VESSELS.
SUPERIOR SHOULDER, LEFT, PUNCH BIOPSY: - BENIGN SKIN WITH MODERATE SOLAR ELASTOSIS, PROMINENT SMALL BLOOD VESSELS AND SCATTERED PERIVASCULAR LYMPHOCYTES AND PLASMA CELLS. - NEGATIVE FOR BASAL CELL CARCINOMA. - NEGATIVE FOR ACTINIC KERATOSIS.
Micro
The sections show hair bearing skin with solar elastosis and numerous small dilated blood vessels. The dermis is mildly fibrotic. Compact keratin is present.
The epidermis matures to the surface. A granular layer is present. There is no basal epidermal atypia. No melanocytic nests are identified. There is no palisading of the basal cells. Rare scattered lymphocytes are in the dermis.
Very common - viral
Verruca vulgaris
- AKA common wart.
General
- Etiology - HPV.
- Very common.
Notes:
- Related to condyloma acuminatum.
Gross
Features:
Images:
Microscopic
Features:[15]
- Hyperkeratosis (more keratin - thick stratum corneum) - in "columns"; keratin in separate towers - not a flat thick sheet.
- Hypergranulosis (thicker stratum granulosum).
- Papillomatous hyperplasia:
- Rete ridge lengthening (~7-10x normal) and thickening.
- Rete ridge curvature toward the centre of the lesion (like the roads to the Palace of Versailles) - important.
- Large blood vessels at the dermal-epidermal junction - between the rete ridges.
- +/-Viral changes - perinuclear halo, nucleus small and hyperchromatic[16] - virtually diagnostic when present.
- +/-Binucleation.
Memory device: there is more of everything - more s. corneum, s. granulosum, s. spinosum, longer rete ridges, more (larger) blood vessels.
DDx:
- Squamous cell carcinoma - nuclear atypia full thickness and often more pronounced.
- Hypertrophic actinic keratosis - often accompanied by solar elastosis.
- Actinic keratosis with superimposed lichen simplex chronicus.[17]
- Seborrheic keratosis - may have focal clear cell changes.
- Condyloma accuminatum - genital region.
Images
www:
Sign out
SKIN LESION, RIGHT LOWER LEG, SHAVE BIOPSY: - VERRUCA VULGARIS.
Micro
The sections show skin with elongated rete ridges, acanthosis, hypergranulosis, hyperkeratosis in vertical columns, focal parakeratosis, dilated blood vessels at the dermal-epidermal junction and koilocytic change. Mild basilar nuclear atypia is present.
Without koilocytes
The sections show skin with elongated rete ridges that curve toward the centre of the lesion, acanthosis, hypergranulosis, hyperkeratosis in vertical columns, and dilated blood vessels at the dermal-epidermal junction. Minimal basilar nuclear enlargement is present. No definite koilocytic change is apparent.
No parakeratosis is identified. Mild solar elastosis is identified. No melanocytic nests are apparent. Mitotic activity is not apparent.
Verruca plana
General
- Common.
- Usu. hands and face.[18]
Microscopic
Features:[18]
- Orthokeratosis with basketweave pattern.
- Hypergranulosis.
- Viral keratohyaline.
- Koilocytes.
- Acanthosis - yet flat surface and base.
Notes:
- It differs from verruca vulgaris... (1) orthokeratosis, (2) flat surface and base.
Less common
Chronic folliculitis
- Folliculitis redirect here.
General
- Common.
- Infrequently biopsied.
Gross
- Erythema.[19]
DDx gross:
Microscopic
Features:
- Inflammation around the hair follicle - key feature.
- Lymphocytes - usu. predominant.
- +/-Chronic changes:
- Acanthosis.
- Hyperkeratosis.
- Hypergranulosis.
DDx:
Sign out
SKIN LESION, UPPER ARM, BIOPSY: - CHRONIC FOLLICULITIS WITH SECONDARY SURFACE CHANGES.
Micro
The sections show hair-bearing skin with abundant lymphocytes around and within the hair follicle wall.
The non-hair follicle epidermis has acanthosis, hypergranulosis and compact hyperkeratosis. There is no inflammatory cell infiltrate in the non-hair follicle epidermis or at the non-hair follicle interface.
There are no granulomas.
Clear cell acanthoma
General
- Benign.
- Elderly.
- Classically on the leg.[20]
- Rare.
- Clinically not distinct.
- Suspected clinically in only ~3% of cases.[21]
Microscopic
Features:[22]
- Psoriasiform pattern - epidermal thickening (acanthosis).
- Keratinocytes:
- Pale or light pink cytoplasm (when compared to surrounding non-lesional keratinocytes).
- Separated from one another (spongiosis).
- +/-Stratum corneum neutrophils.
DDx:
Images:
Chondrodermatitis nodularis chronica helicis
- AKA chondrodermatitis nodularis helicis.
- Abbreviated CNCH.
General
- Tender/painful - key clinical feature.
- Typically right ear - people more often sleep on this one.[23]
- Usually >40 years old.
Etiology:
- Trauma/mechanical.
Gross
- Papule on ear.
- +/-Erythematous.
- +/-Crust.
Clinical DDx:[23]
Images:
Microscopic
Features:[23]
- Dermal inflammation.
- Epithelial hyperlasia.
- Fibrosis.
- Cartilaginous pathology:
- Perichondrial inflammation - key feature.
- Perichondrial disruption.
- +/-Necrosis.
- +/-Hemorrhage.
Images:
Sign out
Superficial biopsy
SKIN LESION, LEFT ANTIHELIX OF EAR, BIOPSY: - SUPERFICIAL SKIN WITH ACANTHOSIS, HYPERKERATOSIS, MODERATE SOLAR ELASTOSIS, HYPERGRANULOSIS AND A MILD LYMPHOCYTIC PERIVASCULAR INFILTRATE. - NO CARTILAGE IS IDENTIFIED. - NEGATIVE FOR DYSPLASIA AND MALIGNANCY. COMMENT: The findings are non-specific. Chondrodermatitis cannot be excluded.
Cutaneous calcinosis
- AKA calcinosis cutis.
General
- Benign in itself; underlying cause may not be benign.
- May be a scrotal lesion - known as scrotal calcinosis.[24]
Subtypes:[25]
- Dystrophic - due to death of cells; may be related to a tumour.
- Metastatic - due to chronic renal failure; hyperkalemia; paraneoplastic phenomenon.
- Iatrogenic - post surgical.
- Idiopathic.
Microscopic
Features:
- Dermal calcification:
- Acellular purple blobs on H&E.
- +/-Artefactual tearing of surrounding tissue due to processing (cutting).
- +/-Small artefactual lines ~1-2 micrometers due to processing (cutting).
- +/-Greyish rim of paucicellular material.
- Usu. well-circumscribed.
- May be surrounded by a palisading granuloma & giant cells.
- Acellular purple blobs on H&E.
Images:
Sign out
SKIN AND SUBCUTANEOUS LESION, LEFT HIP, EXCISION: - SUBCUTANEOUS CALCIFICATION SURROUNDED BY BENIGN FIBROUS TISSUE. - DERMAL SCAR. - NEGATIVE FOR MALIGNANCY.
SUBCUTANEOUS MASS, OVER BURSA OF ELBOW, EXCISION: - CALCINOSIS CUTIS.
Micro
The sections show subcutaneous calcifications surrounded by macrophages and giant cells. No nuclear atypia is apparent. The overlying skin is unremarkable.
Dilated pore of Winer
General
- Benign.
- Looks like zit.
Microscopic
Features:[26]
- Dilated hair follicle with keratin.
- Acanthosis.
- Budding of epidermis (into dermis).
Lichenoid keratosis
General
- Caucasians - middle age or older.
- May be a variant of seborrheic keratosis (with marked inflammation).[27]
Clinical DDx:[27]
- Basal cell carcinoma, squamous cell carcinoma of the skin, melanocytic neoplasm.
Microscopic
Features:[28]
- Hyperkeratosis.
- Parakeratosis.
- Band of inflammatory cells at DE junction (lichenoid inflammation).
- Dead keratinocytes (Civatte bodies).
- Dermal melanophages.
DDx:
- Lichen planus - need clinical correlation (mucosal lesions).
- Drug reaction.
- Cutaneous T-cell lymphoma.
- Regressed melanocytic lesion, esp. malignant melanoma.
- Lichenoid actinic keratosis - has atypical hyperchromatic basal cells - esp. at edge of lesion, usu. in the context of solar elastosis.
Images:
Sign out
SKIN LESION, MID-MIDDLE BACK, PUNCH BIOPSY: - LICHENOID KERATOSIS.
Granuloma annulare
Necrobiosis lipoidica
General
Associated with:
- Diabetes mellitus - known as necrobiosis lipoidica diabeticorum.
- Rheumatoid arthritis.
Gross
Image:
Microscopic
Features:[29]
- Dermal palisading granuloma around:
- Necrotic collagen - key feature.
- Nuclei "missing" - have undergone karyolysis.
- Necrotic collagen - key feature.
- Little mucin, no normal dermis between foci.
- Plasma cells - common.[30]
- May involve adipose tissue.
DDx:
- Granuloma annulare - more mucin, normal dermis between foci,[29] plasma cells uncommon,[30] no fat involvement - usu. more superficial.
- Rheumatoid nodule.
Images
www:
- Necrobiosis lipoidica (dermatology.cdlib.org).
- Necrobiosis lipoidica (drmihm.com).
- Necrobiosis lipoidica (dermnetnz.org).
Keloid
Angiofibroma
- See also: nasopharyngeal angiofibroma.
- Should not be confused with angiokeratoma.
General
- May be seen in the context of tuberous sclerosis - especially "butterfly area of the face".[31]
- Solitary lesions in adults are known as fibrous papules and classically arise on the nose.[32]
Clinical:
- Firm, dome-shaped, flesh coloured.
Microscopic
Features:[31]
- Dome-shaped.
- Fibrotic dermis.
- Enlarged fibroblasts.
- Dilated small vessels.
DDx:
- Benign fibrous papule - solitary, nose lesion.
Image:
Benign fibrous papule
- AKA fibrous papule.
General
- An angiofibroma on the face that is solitary.[32][34]
Gross
Microscopic
Features:[31]
- Dome-shaped.
- Fibrotic dermis.
- Enlarged fibroblasts.
- Dilated small vessels.
- +/-Multinucleated stromal cells.[35]
- +/-Stellate cells.[35]
DDx:
- Angiofibroma - not solitary or not on the nose.
Note:
- Several variants exist.[34]
Sign out
SKIN LESION, CHIN, BIOPSY: - BENIGN FIBROUS PAPULE.
Molluscum contagiosum
- Abbreviated MC.
General
- Etiology: caused by molluscum contagiosum virus.
- May be abundant in immune deficient individuals, e.g. HIV/AIDS.
Gross
Features:[36]
- Dome-shaped papules, flesh coloured or pearly.
- Usually face or trunk.
- +/-Central umbilication.
- Central depression.
DDx - gross:
Image:
Microscopic
Features:[36]
- A suprabasilar epidermal lesion consisting of "molluscum bodies" -- in other words "molluscum bodies" are found above the stratum basale +/- extension to the skin surface.
- Molluscum bodies - key feature:
- Large cells with (granular) eosinophilic cytoplasmic inclusions.
- The inclusions usually fill the cytoplasm.
- Inclusions are usually one per cell... but may be multiple.
- Small peripheral nucleus.
- Large cells with (granular) eosinophilic cytoplasmic inclusions.
- Molluscum bodies - key feature:
- +/-Lymphocytes.
Notes:
- Molluscum bodies very vaguely resemble signet ring cells -- but:
- Cytoplasm is eosinophilic and granular.
- Nucleus usually smaller than in signet ring cells.
- Molluscum bodies are only in the epidermis - an uncommon place to find SRCs without finding them elsewhere.
- The granular eosinophilic cytoplasmic inclusions represents accumulated virons.
- Molluscum bodies "grow" toward the surface
DDx:
- Nothing really - it is very distinctive.
Images:
- Molluscum contagiosum - high mag. (WC).
- Molluscum contagiosum - low magnification (WC).
- Molluscum contagiosum (WC).
Sign out
SKIN LESION ("SKIN TAG"), EXCISION:
- MOLLUSCUM CONTAGIOSUM.
Micro
The section shows fragments of skin with epithelium on three sides. Large suprabasilar cells with eosinophilic intracytoplasmic inclusions (molluscum bodies) and small eccentric nuclei are present, and extend to the skin surface. The epithelium is acanthotic; however, it matures to the surface. There is no significant inflammation.
Superficial dermal infiltrates
Discussed in detail by Alsaad and Ghazarian.[37]
Dermal perivascular lymphoeosinophilic infiltration
- Abbreviated DPLI.
Microscopic appearance is just what it is called:
- Lymphocytes and eosinophils around the vessels in the superficial dermis.
DDx:[37]
- Insect bite - classically wedge-shaped.[38]
- Drug reaction.
- Urticarial reaction.
- Prevesicular early stage of bullous pemphigoid.
- HIV related dermatoses.
Notes:
- May superficially resemble cutaneous lymphoma.[38]
Images:
Congenital dermal melanocytosis
- AKA Mongolian spots.
- Classically seen in asian children.
Gross:
- Brown or blue-grey patch in the lumbosacral area.
Mastocytosis
General
- Abundance of mast cells.
Classification:[39]
- Cutaneous (only) - usually children.
- Urticaria pigmentosa.
- Others.
- Systemic - usually adults.
- Indolent subvariant.
- Aggressive subvariant.
- Leukemic subvariant.
Microscopic
Features:[40]
- Cells in the superficial/mid dermis that are:
- Lymphocyte-like with more cytoplasm that is granular.
- Cells may have spindled or stellate morphology.
- Tend to be more abundant around vessels.
- Lymphocyte-like with more cytoplasm that is granular.
- +/-Eosinophils (common).
- +/-Edema - often prominent; gives cells a white halo.
Notes:
- Lymphocyte vs. mast cell:
- Lymphocytes = round; mast cells = ovoid.
Images:
- www:
- WC:
Stains
- Toluidine blue -- highlights the granules.
IHC
- CD117 +ve.
- Tryptase +ve.[41]
Ichthyosis
General
- Comes in different flavours.
- Usu. inherited... thus a pediatric condition.
Gross
- Fish scale-like appearance.
Image:
Microscopic
Features:[40]
- Thick stratum corneum without basket-weave pattern.
Palmar fibromatosis
General
Clinical:[42]
- Usually older - 60s or 70s (years old).
- Male > female.
- Associated with:
- May be familial.
Gross
- Ring finger - classic location.[citation needed]
- Nodular.
- Poorly demarcated.
Image:
Microscopic
- Poorly demarcated, usu. multiple lesions/multiple nodules.
- Composed of bland spindle cells in dense collagen.
- Pale grey cytoplasm (moderate quantity).
- Pale ovoid nuclei with small round nucleoli.
- Giant cells - rare.
Note:
- No nuclear atypia.
- Mitotic figures - rarely present, none atypical.
- May see Pacinian corpuscle (AKA lamellar corpuscle) as an incidental finding.
DDx:[44]
- Calcifying aponeurotic fibroma - calcification, chondroid differentiation, usu. < 20 years old.
- Extra-abdominal desmoid fibromatosis - extremely rare on hands and feet, muscle infiltrative.
- Inclusion body fibromatosis.
- Fibrosarcoma - atypia, necrosis, herring-bone pattern.
- Synovial sarcoma - one mass.
- Epithelioid sarcoma - necrosis, atypia.
- Metastatic metaplastic carcinoma, e.g. metaplastic breast carcinoma - extremely uncommon.
Images:
- Palmer fibromatosis (biomedsearch.com).[45]
- Palmar fibromatosis (unibas.ch).
- Pacinian corpuscle (WC).
- Tendon without fibromatosis - intermed. mag. (WC).
IHC
- Beta-catenin +ve (cytoplasmic & nuclear).[46]
Sign out
Left
PALMAR FASCIA, LEFT, FASCIECTOMY: - PALMAR FIBROMATOSIS.
Right
PALMAR FASCIA, RIGHT, FASCIECTOMY: - PALMAR FIBROMATOSIS.
Micro
The sections show multiple poorly-demarcated nodules composed of bland spindle cells with moderate pale grey cytoplasm and pale ellipsoid nuclei with small round nucleoli. The poorly-demarcated nodules are completely surrounded by dense collagen. Calcification is not present. There is no nuclear atypia or necrosis. Mitotic activity is not identified. Benign fibroadipose tissue is present.
Missed fibromatosis
PALMAR FASCIA, LEFT, FASCIECTOMY: - PALMAR FASCIA WITHIN NORMAL LIMITS AND BENIGN FIBROADIPOSE TISSUE -- IN AN INDIVIDUAL WITH A CLINICAL HISTORY OF PALMAR FIBROMATOSIS. - NEGATIVE FOR MALIGNANCY.
Micro
The sections show dense collagen (tendon) without an apparent pathology. Calcification is not present. There is no nuclear atypia or necrosis. Mitotic activity is not identified. Benign fibroadipose tissue is present. Lamellar corpuscles are present. The tissue was submitted in toto and levels were cut.
Straight
PALMAR FASCIA, RIGHT, FASCIECTOMY: - PALMAR FASCIA WITHIN NORMAL LIMITS. - NEGATIVE FOR FIBROMATOSIS. COMMENT: The tissue was submitted in toto and levels were cut.
Micro
The sections show dense collagen (tendon) without an apparent pathology. Calcification is not present. There is no nuclear atypia or necrosis. Mitotic activity is not identified. Benign fibroadipose tissue is present. Lamellar corpuscles are present.
Angiomyoma
- Do not confuse with angiomyxoma.
General
- Benign.
- Female > male.[47]
Microscopic
Features:
- Well-circumscribed lesion with fascicular architecture.
- Spindle cells/epithelioid cell with moderate eosinophilic (pink) cytoplasm.
- Thick-walled blood vessels. (???)
Images:
Angiokeratoma
General
- Rare.
- May be seen in the context of Fabry disease.[48]
Notes:
- Shouldn't be confused with angiofibroma which is associated tuberous sclerosis.
Gross
- Dark lesions.
Clinical DDx:
Images
Microscopic
Features:[48]
- Ectatic superficial dermal vessels.
- Overlying hyperkeratosis (thick stratum corneum).
- Should have "epidermal collarette".[49]
- Vascular space surrounded by epidermis on three sides.
Others features:[citation needed]
- Irregular acanthosis.
- Longer rete ridges.
DDx:
Images
www:
Sign out
SKIN LESION, LEFT POPITEAL FOSSA, PUNCH BIOPSY: - ANGIOKERATOMA.
Inverted follicular keratosis
- Abbreviated IFK.[50]
General
- Benign skin lesion.
- Central face - middle age.[51]
- Uncommon.
- May be considered a variant of seborrheic keratosis that is predominantly endophytic.[52]
Microscopic
Features:[51]
- Keratinocyte of cytologically benign proliferation.
- "Squamous eddies" (whorls of keratin).
- Coarse keratohyaline granules.
DDx:
- Squamous cell carcinoma of the skin.
- Trichilemmoma.
- Seborrheic keratosis - has an exophytic component.
Images:
- Inverted follicular keratosis - low mag. (flickr.com).
- Inverted follicular keratosis - high mag. (flickr.com).
- Inverted follicular keratosis - several images (mckeedermpath.com).
Sign out
SKIN LESION, FACE, BIOPSY: - INVERTED FOLLICULAR KERATOSIS.
Micro
The sections show skin with acanthosis, pseudohorn cysts, and focal basal epidermal pigmentation. There is no basal nuclear atypia, no mitoses and there are no melanocytic nests. There is minimal dermal inflammation. There is no apparent solar elastosis.
Focal cutaneous mucinosis
General
- Benign.
- May be associated with systemic disease.[54]
Microscopic
Features:
- Light blue whispy material in the dermis - key feature.
DDx:
- Dermal edema.
- Digital mucous cyst.
Panniculitis
This is dealt with in the panniculitis article.
DDx for panniculitis:
- Erythema nodosum.
- Erythema induratum.
- Self-inflicted trauma.
- Systemic lupus erythematosus.
- Weird stuff.
Rare
Necrotizing fasciitis
- Not to be confused with nodular fasciitis.
- AKA flesh-eating disease.
General
- High mortality.
- May be diagnosed at frozen section.[55]
- Classically associated with Group A streptococcus.
Treatment:
- Operative debridement.
Microscopic
Features:
Note:
- Fat lobules between septae may be normal.
DDx:
Images:
Porokeratosis
General
- Genetic.
- Several subtypes.
Notes:
- Not the same as punctate porokeratotic keratoderma.[57]
Microscopic
Features:
- Cornoid lamella (pathognomonic) - key feature:
- Compact keratosis over a hair follicle.
- +/-Rete ridge loss.
Images:
Nevus sebaceous
- AKA nevus sebaceous of Jadassohn.
General
- Congenital - considered a hamartoma.[58]
- Usually sporadic - may be transmitted autosomal dominant.[58]
- Malignant tumours may arise within a nevus sebaceous.
Gross
- Head and neck plaque or papule with:
- Well-circumscribed borders.
- Waxy, yellow appearance.
- Area usu. devoid of hair.[60]
DDx - gross:
Image:
Microscopic
Features:[59]
- Abundant sebaceous glands.
- Immature/abortive hair follicles.
- No normal terminal hair follicles.
- Papillomatous epidermal hyperplasia.
Images:
Nevus lipomatosus superficialis
- Abbreviated NLS.
- AKA nevus lipomatosus cutaneous superficialis, abbreviated NLCS.
- AKA nevus lipomatosus.[61]
General
Clinically separated into:[64]
- Solitary - one lesion.
- Multiple - more than one lesion.
Gross
Features:[62]
- Pedunculated lesion.
- Soft.
- Usually lower trunk or gluteal region.[65]
Image:
Microscopic
Features:[66]
- Benign adipose tissue in the dermis.
- Adipocytes in reticular dermis +/- papillary dermis.[67]
DDx:
- Lipoma.
- Fibroepithelial polyp (skin tag).
- Intradermal nevus with adipocytes.[68]
Images:
- NLS (dermamin.com).[69]
- NLS (humpath.com).[70]
- NLS (nih.gov).[62]
- Nevus lipomatosus (dermpedia.org).
Sign out
SKIN LESION ("SKIN TAG"), LEFT HIP, EXCISION:
- NEVUS LIPOMATOSUS SUPERFICIALIS.
Bullous disease
Cysts
See also
References
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 26. ISBN 978-0443066542.
- ↑ URL: http://www.pediatrics.wisc.edu/education/derm/text.html. Accessed on: 23 August 2012.
- ↑ URL: http://missinglink.ucsf.edu/lm/DermatologyGlossary/tinea.html. Accessed on: 25 February 2013.
- ↑ Mitchell, Richard; Kumar, Vinay; Fausto, Nelson; Abbas, Abul K.; Aster, Jon (2011). Pocket Companion to Robbins & Cotran Pathologic Basis of Disease (8th ed.). Elsevier Saunders. pp. 596. ISBN 978-1416054542.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 342. ISBN 978-0443066542.
- ↑ URL: http://dermatlas.med.jhmi.edu/derm/result.cfm?Diagnosis=1196583692. Accessed on: 1 September 2011.
- ↑ URL: http://dermatology-s10.cdlib.org/143/case_presentations/skintags/allegue.html. Accessed on: 9 January 2013.
- ↑ Picascia, DD.; Robinson, JK. (Aug 1987). "Actinic cheilitis: a review of the etiology, differential diagnosis, and treatment.". J Am Acad Dermatol 17 (2 Pt 1): 255-64. PMID 3305604.
- ↑ Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1188. ISBN 978-1416031215.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 76. ISBN 978-0443066542.
- ↑ 11.0 11.1 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 77. ISBN 978-0443066542.
- ↑ URL: http://www.dermnetnz.org/dermal-infiltrative/solar-elastosis.html. Accessed on: 27 March 2013.
- ↑ Thomas, NE.; Kricker, A.; From, L.; Busam, K.; Millikan, RC.; Ritchey, ME.; Armstrong, BK.; Lee-Taylor, J. et al. (Nov 2010). "Associations of cumulative sun exposure and phenotypic characteristics with histologic solar elastosis.". Cancer Epidemiol Biomarkers Prev 19 (11): 2932-41. doi:10.1158/1055-9965.EPI-10-0686. PMID 20802019.
- ↑ 14.0 14.1 Karagas, MR.; Zens, MS.; Nelson, HH.; Mabuchi, K.; Perry, AE.; Stukel, TA.; Mott, LA.; Andrew, AS. et al. (Mar 2007). "Measures of cumulative exposure from a standardized sun exposure history questionnaire: a comparison with histologic assessment of solar skin damage.". Am J Epidemiol 165 (6): 719-26. doi:10.1093/aje/kwk055. PMID 17204514.
- ↑ URL: http://missinglink.ucsf.edu/lm/DermatologyGlossary/verruca_vulgaris.html. Accessed on: 14 July 2010.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 106-7. ISBN 978-0443066542.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 353. ISBN 978-0443066542.
- ↑ 18.0 18.1 Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 480. ISBN 978-0781765275.
- ↑ URL: http://www.webmd.com/skin-problems-and-treatments/tc/folliculitis-topic-overview. Accessed on: 7 November 2012.
- ↑ Akin, FY.; Ertam, I.; Ceylan, C.; Kazandi, A.; Ozdemir, F.. "Clear cell acanthoma: new observations on dermatoscopy.". Indian J Dermatol Venereol Leprol 74 (3): 285-7. PMID 18583817.
- ↑ Morrison, LK.; Duffey, M.; Janik, M.; Shamma, HN. (Sep 2010). "Clear cell acanthoma: a rare clinical diagnosis prior to biopsy.". Int J Dermatol 49 (9): 1008-11. PMID 20931670.
- ↑ URL: http://www.drmihm.com/cases/case.cfm?CaseID=45. Accessed on: 7 February 2012.
- ↑ 23.0 23.1 23.2 Devani, A.; Barankin, B. (May 2007). "Dermacase. Chondrodermatitis nodularis chronica helicis.". Can Fam Physician 53 (5): 821, 837. PMID 17879469.
- ↑ Dubey, S.; Sharma, R.; Maheshwari, V. (2010). "Scrotal calcinosis: idiopathic or dystrophic?". Dermatol Online J 16 (2): 5. PMID 20178701.
- ↑ URL: http://emedicine.medscape.com/article/1103137-overview. Accessed on: 21 September 2011.
- ↑ Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 486. ISBN 978-0781765275.
- ↑ 27.0 27.1 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 346. ISBN 978-0443066542.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 347. ISBN 978-0443066542.
- ↑ 29.0 29.1 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 51. ISBN 978-0443066542.
- ↑ 30.0 30.1 URL: http://dermnetnz.org/pathology/necrobiosis-lipoidica-path.html. Accessed on: 24 January 2012.
- ↑ 31.0 31.1 31.2 Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 492. ISBN 978-0781765275.
- ↑ 32.0 32.1 32.2 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 505. ISBN 978-0443066542.
- ↑ URL: http://www.drdittmar.lu/Services.aspx. Accessed on: 1 September 2011.
- ↑ 34.0 34.1 34.2 Jacyk, WK.; Rütten, A.; Requena, L. (2008). "Fibrous papule of the face with granular cells.". Dermatology 216 (1): 56-9. doi:10.1159/000109359. PMID 18032900.
- ↑ 35.0 35.1 Ragaz, A.; Berezowsky, V. (1979). "Fibrous papule of the face. A study of five cases by electron microscopy.". Am J Dermatopathol 1 (4): 353-6. PMID 543528.
- ↑ 36.0 36.1 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 115. ISBN 978-0443066542.
Cite error: Invalid
<ref>tag; name "Ref_Derm115" defined multiple times with different content - ↑ 37.0 37.1 Alsaad, KO.; Ghazarian, D. (Dec 2005). "My approach to superficial inflammatory dermatoses.". J Clin Pathol 58 (12): 1233-41. doi:10.1136/jcp.2005.027151. PMID 16311340.
- ↑ 38.0 38.1 Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Nelso Fausto; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease (7th ed.). St. Louis, Mo: Elsevier Saunders. pp. 1269. ISBN 0-7216-0187-1.
- ↑ Arock, M.; Valent, P. (Aug 2010). "Pathogenesis, classification and treatment of mastocytosis: state of the art in 2010 and future perspectives.". Expert Rev Hematol 3 (4): 497-516. doi:10.1586/ehm.10.42. PMID 21083038.
- ↑ 40.0 40.1 Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1185. ISBN 978-1416031215.
- ↑ Rudzki, Z.; Sotlar, K.; Kudela, A.; Starzak-Gwóźdź, J.; Horny, HP. (2011). "Systemic mastocytosis (SM) and associated malignant bone marrow histiocytosis - a hitherto undescribed form of SM-AHNMD.". Pol J Pathol 62 (2): 101-4. PMID 21866466.
- ↑ URL: http://www.humpath.com/palmar-fibromatosis. Accessed on: 6 January 2011.
- ↑ URL: http://surgpathcriteria.stanford.edu/softfib/plantar_fibromatosis/printable.html. Accessed on: 6 January 2011.
- ↑ 44.0 44.1 URL: http://surgpathcriteria.stanford.edu/softfib/palmar_fibromatosis/differentialdiagnosis.html. Accessed on: 9 November 2012.
- ↑ Wang L, Zhu H (2006). "Clonal analysis of palmar fibromatosis: a study whether palmar fibromatosis is a real tumor". J Transl Med 4: 21. doi:10.1186/1479-5876-4-21. PMC 1488873. PMID 16696857. http://www.biomedsearch.com/nih/Clonal-analysis-palmar-fibromatosis-study/16696857.html.
- ↑ Degreef, I.; De Smet, L.; Sciot, R.; Cassiman, JJ.; Tejpar, S. (Mar 2009). "Beta-catenin overexpression in Dupuytren's disease is unrelated to disease recurrence.". Clin Orthop Relat Res 467 (3): 838-45. doi:10.1007/s11999-008-0590-z. PMID 18958538.
- ↑ Katenkamp D, Kosmehl H, Langbein L (1988). "[Angiomyoma. A pathologo-anatomic analysis of 229 cases]" (in German). Zentralbl Allg Pathol 134 (4-5): 423–33. PMID 3201831.
- ↑ 48.0 48.1 Karen, JK.; Hale, EK.; Ma, L. (2005). "Angiokeratoma corporis diffusum (Fabry disease).". Dermatol Online J 11 (4): 8. PMID 16403380.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 548. ISBN 978-0443066542.
- ↑ Shih, CC.; Yu, HS.; Tung, YC.; Tsai, KB.; Cheng, ST. (Jan 2001). "Inverted follicular keratosis.". Kaohsiung J Med Sci 17 (1): 50-4. PMID 11411260.
- ↑ 51.0 51.1 51.2 Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 387. ISBN 978-0443066542.
- ↑ Busam, Klaus J. (2009). Dermatopathology: A Volume in the Foundations in Diagnostic Pathology Series (1st ed.). Saunders. pp. 341. ISBN 978-0443066542.
- ↑ URL: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC475744/. Accessed on: 11 May 2010.
- ↑ Gandhi, V.; Dogra, D.; Pandhi, RK.. "Cutaneous focal mucinosis.". Indian J Dermatol Venereol Leprol 62 (4): 260-1. PMID 20948074.
- ↑ Majeski, J.; Majeski, E. (Nov 1997). "Necrotizing fasciitis: improved survival with early recognition by tissue biopsy and aggressive surgical treatment.". South Med J 90 (11): 1065-8. PMID 9386043.
- ↑ Wong, CH.; Wang, YS. (Apr 2005). "The diagnosis of necrotizing fasciitis.". Curr Opin Infect Dis 18 (2): 101-6. PMID 15735411.
- ↑ Alikhan, A.; Burns, T.; Zargari, O. (2010). "Punctate porokeratotic keratoderma.". Dermatol Online J 16 (1): 13. PMID 20137755.
- ↑ 58.0 58.1 58.2 West, C.; Narahari, S.; Kwatra, S.; Feldman, S. (Nov 2012). "Autosomal dominant transmission of nevus sebaceous of Jadassohn.". Dermatol Online J 18 (11): 17. PMID 23217958.
- ↑ 59.0 59.1 Simi, CM.; Rajalakshmi, T.; Correa, M.. "Clinicopathologic analysis of 21 cases of nevus sebaceus: a retrospective study.". Indian J Dermatol Venereol Leprol 74 (6): 625-7. PMID 19171988.
- ↑ Kim, JH.; Park, HY.; Ahn, SK. (Oct 2011). "Nevus sebaceous accompanying secondary neoplasms and unique histopathologic findings.". Ann Dermatol 23 (Suppl 2): S231-4. doi:10.5021/ad.2011.23.S2.S231. PMID 22148058.
- ↑ Kaw, P.; Carlson, A.; Meyer, DR. (Jan 2005). "Nevus lipomatosus (pedunculated lipofibroma) of the eyelid.". Ophthal Plast Reconstr Surg 21 (1): 74-6. PMID 15677959.
- ↑ 62.0 62.1 62.2 62.3 Goucha, S.; Khaled, A.; Zéglaoui, F.; Rammeh, S.; Zermani, R.; Fazaa, B. (Dec 2011). "Nevus lipomatosus cutaneous superficialis: Report of eight cases.". Dermatol Ther (Heidelb) 1 (2): 25-30. doi:10.1007/s13555-011-0006-y. PMC 3437641. PMID 22984661. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3437641/.
- ↑ URL: http://www.dermpedia.org/dermpedia-textbook/nevus-lipomatosus. Accessed on: 8 January 2013.
- ↑ Triki, S.; Mekni, A.; Haouet, S.; Mokni, M.; Kchir, N.; Ben Osman Dhahri, A.; Zitouna, M. (Dec 2006). "[Nevus lipomatosus cutaneous superficialis: a clinico-pathological study of 13 cases].". Tunis Med 84 (12): 800-2. PMID 17288284.
- ↑ Jones, EW.; Marks, R.; Pongsehirun, D. (Aug 1975). "Naevus superficialis lipomatosus. A clinicopathological report of twenty cases.". Br J Dermatol 93 (2): 121-33. PMID 1235780.
- ↑ Yap, FB. (May 2009). "Nevus lipomatosus superficialis.". Singapore Med J 50 (5): e161-2. PMID 19495497.
- ↑ Ghosh, SK.; Bandyopadhyay, D.; Jamadar, NS. (2010). "Nevus lipomatosus cutaneous superficialis: An unusual presentation.". Dermatol Online J 16 (7): 12. PMID 20673540.
- ↑ Eng, W.; Cohen, PR. (Nov 1998). "Nevus with fat: clinical characteristics of 100 nevi containing mature adipose cells.". J Am Acad Dermatol 39 (5 Pt 1): 704-11. PMID 9810886.
- ↑ URL: http://www.dermaamin.com/site/histopathology-of-the-skin/66-n/1971-nevus-lipomatosus-superficialis----.html. Accessed on: 7 March 2012.
- ↑ URL: http://www.humpath.com/spip.php?article8134. Accessed on: 17 December 2012.