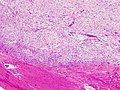
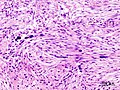
Nodular fasciitis
Jump to navigation
Jump to search
| Nodular fasciitis | |
|---|---|
| Diagnosis in short | |
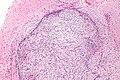
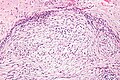
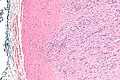
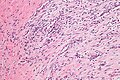
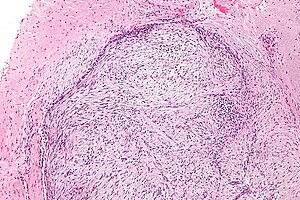 Nodular fasciitis. H&E stain. | |
|
| |
| LM | usu. well-circumscribed, clusters of (non-pleomorphic) spindle cells, inflammation (lymphocytes), microcysts in cellular regions - uncommon, mitoses - common, extravasated RBCs. |
| LM DDx | myxoid dermatofibrosarcoma protuberans, cellular dermatofibroma, desmoid-type fibromatosis, other spindle cell lesions of the skin |
| IHC | CD34 -ve, desmin -ve, SMA -ve, S-100 -ve, AE1/AE3 -ve. |
| Molecular | t(15;15) ? |
| Gross | usu. upper extremity ~45% of cases |
| Site | soft tissue - fibroblastic/myofibroblastic tumours |
|
| |
| Clinical history | associated with trauma |
| Prevalence | common soft tissue lesion |
| Prognosis | benign |
Nodular fasciitis is a benign soft tissue lesion.
It should not to be confused with necrotizing fasciitis.
General
- Benign.
- All age groups - though typically 20-40 years old.
- Associated with trauma.
- Often rapidily growing - clinically concerning for malignancy.[1]
- Commonly misdiagnosed as malignant.[2]
Subtypes - location:[2]
- Subcutaneous.
- Intramuscular.
- Fascial
- Dermal - rare.
- Intravascular - rare.
Gross
- Usually upper extremity ~45% of cases.[2]
- Other locations in order: trunk (~20%), head and neck (~20%), and lower extremities (~15%).
Microscopic
- Usu. well-circumscribed.
- Clusters of (non-pleomorphic) spindle cells.
- Inflammation (lymphocytes).
- Microcysts in cellular regions - uncommon - discriminatory.
- Mitoses - common.
- Extravasated RBCs.
- Tissue culture-like/CNS-like morphology.
- Thick (keloid-like) collagen bundles - key feature.
- Extravasated RBCs.
- Inflammation.
- +/-Giant cells.
Notes:
- No significant nuclear atypia.
- No atypical mitoses.
- May be cellular.
DDx:[7]
- Myxoid dermatofibrosarcoma protuberans.
- Cellular dermatofibroma.
- Desmoid-type fibromatosis.
- Other spindle cell lesions of the skin.
Images
www:
IHC
Routine spindle cell panel:
- CD34 -ve.
- Desmin -ve.
- SMA +ve -- strong.[citation needed]
- S-100 -ve.
- AE1/AE3 -ve.
Others:
- H-caldesmon -ve.
- EMA -ve.
- Vimentin +ve.
Molecular
- Evolving - case reports.
- t(15;15)(q13;q25).[8]
See also
References
- ↑ Chi, CC.; Kuo, TT.; Wang, SH. (Aug 2003). "Nodular fasciitis: clinical characteristics and preoperative diagnosis.". J Formos Med Assoc 102 (8): 586-9. PMID 14569327.
- ↑ 2.0 2.1 2.2 Dinauer, PA.; Brixey, CJ.; Moncur, JT.; Fanburg-Smith, JC.; Murphey, MD.. "Pathologic and MR imaging features of benign fibrous soft-tissue tumors in adults.". Radiographics 27 (1): 173-87. doi:10.1148/rg.271065065. PMID 17235006.
- ↑ Humphrey, Peter A; Dehner, Louis P; Pfeifer, John D (2008). The Washington Manual of Surgical Pathology (1st ed.). Lippincott Williams & Wilkins. pp. 606. ISBN 978-0781765275.
- ↑ de Feraudy S, Fletcher CD (September 2010). "Intradermal nodular fasciitis: a rare lesion analyzed in a series of 24 cases". Am. J. Surg. Pathol. 34 (9): 1377–81. doi:10.1097/PAS.0b013e3181ed7374. PMID 20716998.
- ↑ Dickson, B. 26 April 2011.
- ↑ URL: http://anvita.info/wiki/Nodular_Fasciitis. Accessed on: 11 November 2011.
- ↑ URL: http://www.mckeedermpath.com/SPOT%20DIAGNOSIS%20CASE%20268.html. Accessed on: 11 November 2011.
- ↑ Velagaleti GV, Tapper JK, Panova NE, Miettinen M, Gatalica Z (March 2003). "Cytogenetic findings in a case of nodular fasciitis of subclavicular region". Cancer Genet. Cytogenet. 141 (2): 160–3. PMID 12606136.