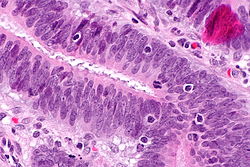
Lynch syndrome
Jump to navigation
Jump to search
The printable version is no longer supported and may have rendering errors. Please update your browser bookmarks and please use the default browser print function instead.
Lynch syndrome, also hereditary non-polyposis colorectal cancer syndrome (abbreviated HNPCC), is a constellation of clinical findings caused by a mutation in a mismatch repair gene, of which there are several.[1]
As the name suggests, HNPCC is a form of inherited colorectal cancer that is not characterized by abundant intestinal polyps (non-polyposis), as in adenomatous polyposis coli.
The term Lynch syndrome is preferred as individuals with this syndrome often present with non-colorectal cancers.
General
- Definitive diagnosis is by molecular testing (sequencing).
- Immunohistochemical stains have a very strong concordance with molecular testing - see microsatellite instability.
Clinical classification
Divided into:[1]
- Lynch syndrome I - colon cancer associated.
- Lynch syndrome II - non-colon cancer associated.
- More common in females (~50%) vs. males (~25%).[2]
Genes
- MSH2 gene[1] - most common.
- MLH1 gene[3] - second most common.
- PMS2 gene.[4]
- MSH6 gene[5] - tend to present in older individuals compared to individuals with MLH1 or MSH2 mutations.[6]
- Others.
Associations
- Colorectal carcinoma.
- Endometrial carcinoma.
- Morphologic features are not sensitive - IHC required.
- Non-endometrioid endometrial carcinoma,[7] e.g. endometrial clear cell carcinoma.[8]
- Endometrioid endometrial carcinoma.[9]
- Suggestive features: lower uterine segment, tumour infiltrating lymphocytes.[10]
- Stomach carcinoma,[1] intestinal-type.[11]
- Biliary tree carcinoma.[1]
- Pancreatic carcinoma.[1]
- Urinary system carcinoma.[1]
Lame mnemonic GP CUBE:
- Gastric.
- Pancreas.
- CRC.
- UCC.
- Biliary.
- Endometrial.
Note:
- All the cancers are below the diaphragm.
Special types
Muir-Torre syndrome
- Abbreviated MTS.
- Muir-Torre syndrome is a subset of HNPCC that includes the presence of sebaceous adenomas,[16] and sebaceous carcinomas.[17]
- Cutaneous pathology precedes the internal malignancy in ~40% of cases.[17]
Molecular pathology:
- MTS is caused by mutations in MSH2 or MLH1.[18]
IHC
See also
References
- ↑ 1.0 1.1 1.2 1.3 1.4 1.5 1.6 Online 'Mendelian Inheritance in Man' (OMIM) 120435
- ↑ 2.0 2.1 Barrow, E.; Robinson, L.; Alduaij, W.; Shenton, A.; Clancy, T.; Lalloo, F.; Hill, J.; Evans, DG. (Feb 2009). "Cumulative lifetime incidence of extracolonic cancers in Lynch syndrome: a report of 121 families with proven mutations.". Clin Genet 75 (2): 141-9. doi:10.1111/j.1399-0004.2008.01125.x. PMID 19215248.
- ↑ Online 'Mendelian Inheritance in Man' (OMIM) 120436
- ↑ Online 'Mendelian Inheritance in Man' (OMIM) 600259
- ↑ Online 'Mendelian Inheritance in Man' (OMIM) 600678
- ↑ Stewart, A. (2013). "Genetic testing strategies in newly diagnosed endometrial cancer patients aimed at reducing morbidity or mortality from lynch syndrome in the index case or her relatives.". PLoS Curr 5. doi:10.1371/currents.eogt.b59a6e84f27c536e50db4e46aa26309c. PMID 24056992.
- ↑ Okuda T, Sekizawa A, Purwosunu Y, et al. (2010). "Genetics of endometrial cancers". Obstet Gynecol Int 2010: 984013. doi:10.1155/2010/984013. PMC 2852605. PMID 20396392. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2852605/.
- ↑ Garg, K.; Soslow, RA. (Aug 2009). "Lynch syndrome (hereditary non-polyposis colorectal cancer) and endometrial carcinoma.". J Clin Pathol 62 (8): 679-84. doi:10.1136/jcp.2009.064949. PMID 19638537. http://jcp.bmj.com/content/62/8/679.long.
- ↑ Lax, SF. (Jan 2002). "[Dualistic model of molecular pathogenesis in endometrial carcinoma].". Zentralbl Gynakol 124 (1): 10-6. doi:10.1055/s-2002-20303. PMID 11873308.
- ↑ Garg, K.; Soslow, RA. (Aug 2009). "Lynch syndrome (hereditary non-polyposis colorectal cancer) and endometrial carcinoma.". J Clin Pathol 62 (8): 679-84. doi:10.1136/jcp.2009.064949. PMID 19638537.
- ↑ Cristofaro, G.; Lynch, HT.; Caruso, ML.; Attolini, A.; DiMatteo, G.; Giorgio, P.; Senatore, S.; Argentieri, A. et al. (Jul 1987). "New phenotypic aspects in a family with Lynch syndrome II.". Cancer 60 (1): 51-8. PMID 3581033.
- ↑ Renkonen-Sinisalo, L.; Sipponen, P.; Aarnio, M.; Julkunen, R.; Aaltonen, LA.; Sarna, S.; Järvinen, HJ.; Mecklin, JP. (May 2002). "No support for endoscopic surveillance for gastric cancer in hereditary non-polyposis colorectal cancer.". Scand J Gastroenterol 37 (5): 574-7. PMID 12059060.
- ↑ Crockett, DG.; Wagner, DG.; Holmäng, S.; Johansson, SL.; Lynch, HT. (May 2011). "Upper urinary tract carcinoma in Lynch syndrome cases.". J Urol 185 (5): 1627-30. doi:10.1016/j.juro.2010.12.102. PMID 21419447.
- ↑ 14.0 14.1 Hartmann, A.; Dietmaier, W.; Hofstädter, F.; Burgart, LJ.; Cheville, JC.; Blaszyk, H. (Mar 2003). "Urothelial carcinoma of the upper urinary tract: inverted growth pattern is predictive of microsatellite instability.". Hum Pathol 34 (3): 222-7. doi:10.1053/hupa.2003.22. PMID 12673555.
- ↑ van der Post, RS.; Kiemeney, LA.; Ligtenberg, MJ.; Witjes, JA.; Hulsbergen-van de Kaa, CA.; Bodmer, D.; Schaap, L.; Kets, CM. et al. (Jul 2010). "Risk of urothelial bladder cancer in Lynch syndrome is increased, in particular among MSH2 mutation carriers.". J Med Genet 47 (7): 464-70. doi:10.1136/jmg.2010.076992. PMID 20591884.
- ↑ Kumar, Vinay; Abbas, Abul K.; Fausto, Nelson; Aster, Jon (2009). Robbins and Cotran pathologic basis of disease (8th ed.). Elsevier Saunders. pp. 1177. ISBN 978-1416031215.
- ↑ 17.0 17.1 Cohen, PR.; Kohn, SR.; Kurzrock, R. (May 1991). "Association of sebaceous gland tumors and internal malignancy: the Muir-Torre syndrome.". Am J Med 90 (5): 606-13. PMID 2029018.
- ↑ Online 'Mendelian Inheritance in Man' (OMIM) 158320