Difference between revisions of "Lymph node metastasis"
Jump to navigation
Jump to search
(redirect to LN path. article) |
(split out) |
||
| Line 1: | Line 1: | ||
# | '''Lymph node metastasis''' is [[cancer]] that has spread to a [[lymph node]]. | ||
==General== | |||
*Determination of ''lymph node status'' is one of the most common indications for the examination of lymph nodes. | |||
*It is a good idea to look at the tumour (if available) ...before looking at the LNs for mets. | |||
*Lymph node metastasis, in the absence of other metastases, often up-stage a cancer from [[cancer staging|stage]] II to stage III. | |||
==Gross== | |||
*Outside: | |||
**"Large" - size varies by site. | |||
***Neck >10 mm.<ref name=pmid18337039>{{Cite journal | last1 = Mack | first1 = MG. | last2 = Rieger | first2 = J. | last3 = Baghi | first3 = M. | last4 = Bisdas | first4 = S. | last5 = Vogl | first5 = TJ. | title = Cervical lymph nodes. | journal = Eur J Radiol | volume = 66 | issue = 3 | pages = 493-500 | month = Jun | year = 2008 | doi = 10.1016/j.ejrad.2008.01.019 | PMID = 18337039 }}</ref> | |||
**Shape - round more suspicious than oval. | |||
*Sectioned: | |||
**White firm lesion with irregular border - classic appearance. | |||
**Non-fatty hilum.<ref name=pmid18337039/> | |||
==Microscopic== | |||
Features: | |||
*Foreign cell population - '''key feature'''. | |||
**Classic location: subcapsular sinuses. | |||
*+/-Cells with cytologic features of malignancy. | |||
**Nuclear pleomorphism (variation in size, shape and staining). | |||
**Nuclear atypia: | |||
***Nuclear enlargement. | |||
***Irregular nuclear membrane. | |||
***Irregular chromatin pattern, esp. asymmetry. | |||
***Large or irregular nucleolus. | |||
**Abundant mitotic figures. | |||
*+/-Cells in architectural arrangements seen in malignancy; highly variable - dependent on tumour type and differentiation. | |||
**+/-Gland formation. | |||
**+/-Single cells. | |||
**+/-Small clusters of cells. | |||
Notes: | |||
#Cytologic features of malignancy may not be present; some tumours, e.g. gallbladder carcinoma, do not always have overt cytologic features of malignancy. | |||
#*The diagnosis is based on the fact that they are foreign to the lymph node ''and'' architecturally consistent with a well-differentiated malignancy. | |||
#[[Soft_tissue_lesions#Lymph_node_metastases_in_sarcomas|Lymph node metastases in sarcomas]] are uncommon; they are seen in <3% of cases.<ref name=pmid8424704>{{Cite journal | last1 = Fong | first1 = Y. | last2 = Coit | first2 = DG. | last3 = Woodruff | first3 = JM. | last4 = Brennan | first4 = MF. | title = Lymph node metastasis from soft tissue sarcoma in adults. Analysis of data from a prospective database of 1772 sarcoma patients. | journal = Ann Surg | volume = 217 | issue = 1 | pages = 72-7 | month = Jan | year = 1993 | doi = | PMID = 8424704 | PMC = 1242736}}</ref> | |||
#Fatty lymph nodes (esp. fatty hilus<ref name=pmid18337039>{{Cite journal | last1 = Mack | first1 = MG. | last2 = Rieger | first2 = J. | last3 = Baghi | first3 = M. | last4 = Bisdas | first4 = S. | last5 = Vogl | first5 = TJ. | title = Cervical lymph nodes. | journal = Eur J Radiol | volume = 66 | issue = 3 | pages = 493-500 | month = Jun | year = 2008 | doi = 10.1016/j.ejrad.2008.01.019 | PMID = 18337039 }}</ref>) are less likely to harbor metastases.<ref name=pmid21972135>{{Cite journal | last1 = Korteweg | first1 = MA. | last2 = Veldhuis | first2 = WB. | last3 = Mali | first3 = WP. | last4 = Diepstraten | first4 = SC. | last5 = Luijten | first5 = PR. | last6 = van den Bosch | first6 = MA. | last7 = Eijkemans | first7 = RM. | last8 = van Diest | first8 = PJ. | last9 = Klomp | first9 = DW. | title = Investigation of lipid composition of dissected sentinel lymph nodes of breast cancer patients by 7T proton MR spectroscopy. | journal = J Magn Reson Imaging | volume = 35 | issue = 2 | pages = 387-92 | month = Feb | year = 2012 | doi = 10.1002/jmri.22820 | PMID = 21972135 }}</ref> | |||
DDx - mimics of metastatic disease: | |||
*[[Endometriosis]]. | |||
*Ectopic [[decidua]].<ref name=pmid15859655>{{Cite journal | last1 = Wu | first1 = DC. | last2 = Hirschowitz | first2 = S. | last3 = Natarajan | first3 = S. | title = Ectopic decidua of pelvic lymph nodes: a potential diagnostic pitfall. | journal = Arch Pathol Lab Med | volume = 129 | issue = 5 | pages = e117-20 | month = May | year = 2005 | doi = 10.1043/1543-2165(2005)129e117:EDOPLN2.0.CO;2 | PMID = 15859655 }}</ref> | |||
*[[Endosalpingiosis]].<ref name=pmid20631604>{{Cite journal | last1 = Corben | first1 = AD. | last2 = Nehhozina | first2 = T. | last3 = Garg | first3 = K. | last4 = Vallejo | first4 = CE. | last5 = Brogi | first5 = E. | title = Endosalpingiosis in axillary lymph nodes: a possible pitfall in the staging of patients with breast carcinoma. | journal = Am J Surg Pathol | volume = 34 | issue = 8 | pages = 1211-6 | month = Aug | year = 2010 | doi = 10.1097/PAS.0b013e3181e5e03e | PMID = 20631604 }}</ref> | |||
*Melanocytic nevus - intracapsular or within the trabeculae.<ref name=pmid12717252>{{Cite journal | last1 = Biddle | first1 = DA. | last2 = Evans | first2 = HL. | last3 = Kemp | first3 = BL. | last4 = El-Naggar | first4 = AK. | last5 = Harvell | first5 = JD. | last6 = White | first6 = WL. | last7 = Iskandar | first7 = SS. | last8 = Prieto | first8 = VG. | title = Intraparenchymal nevus cell aggregates in lymph nodes: a possible diagnostic pitfall with malignant melanoma and carcinoma. | journal = Am J Surg Pathol | volume = 27 | issue = 5 | pages = 673-81 | month = May | year = 2003 | doi = | PMID = 12717252 }}</ref> | |||
*[[Dermatopathic lymphadenopathy]].{{fact}} | |||
*[[Sinus histiocytosis]] - especially for the junior resident. | |||
*[[Tumour deposit]] (discoutinuous extramural extension) - definition dependent on primary tumour (e.g. in the head & neck they are tumour replaced lymph nodes, in the colon they are considered separate and not counted as lymph nodes). | |||
===Images=== | |||
<gallery> | |||
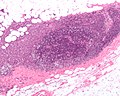
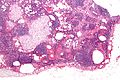
Image:Breast_carcinoma_in_a_lymph_node.jpg | Breast carcinoma LN metastasis (WC) | |||
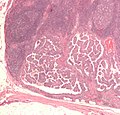
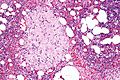
Image:Lymph_node_with_papillary_thyroid_carcinoma.jpg | Thyroid carcinoma LN metastasis (WC) | |||
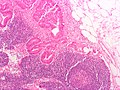
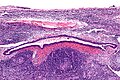
Image:Crc_met_to_node1.jpg | Colorectal carcinoma LN metastasis (WC) | |||
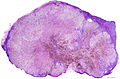
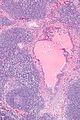
Image:Lymph_node_with_metastatic_melanoma_-_by_Gabriel_Caponetti,_MD.jpg | Melanoma in a lymph node. (WC) | |||
</gallery> | |||
====Mimics==== | |||
<gallery> | |||
Image:Decidua_in_a_lymph_node_-_low_mag.jpg | Decidua in a LN - low mag. (WC) | |||
Image:Decidua_in_a_lymph_node_-_high_mag.jpg | Decidua in a LN - high mag. (WC) | |||
Image:Endometriosis_lymph_node_-_2_-_intermed_mag.jpg | Endometriosis in a LN - intermed. mag. (WC) | |||
Image:Endosalpingiosis_in_lymph_node_-_intermed_mag.jpg | Endosalpingiosis in a LN - intermed. mag. (WC) | |||
Image:Endosalpingiosis_in_lymph_node_-_very_high_mag.jpg | Endosalpingiosis in a LN - very high mag. (WC) | |||
</gallery> | |||
==See also== | |||
*[[Lymph node pathology]]. | |||
*[[Cancer]]. | |||
*[[Cancer staging]]. | |||
==References== | |||
{{Reflist|2}} | |||
[[Category:Lymph node pathology]] | |||
Revision as of 03:08, 10 January 2014
Lymph node metastasis is cancer that has spread to a lymph node.
General
- Determination of lymph node status is one of the most common indications for the examination of lymph nodes.
- It is a good idea to look at the tumour (if available) ...before looking at the LNs for mets.
- Lymph node metastasis, in the absence of other metastases, often up-stage a cancer from stage II to stage III.
Gross
- Outside:
- "Large" - size varies by site.
- Neck >10 mm.[1]
- Shape - round more suspicious than oval.
- "Large" - size varies by site.
- Sectioned:
- White firm lesion with irregular border - classic appearance.
- Non-fatty hilum.[1]
Microscopic
Features:
- Foreign cell population - key feature.
- Classic location: subcapsular sinuses.
- +/-Cells with cytologic features of malignancy.
- Nuclear pleomorphism (variation in size, shape and staining).
- Nuclear atypia:
- Nuclear enlargement.
- Irregular nuclear membrane.
- Irregular chromatin pattern, esp. asymmetry.
- Large or irregular nucleolus.
- Abundant mitotic figures.
- +/-Cells in architectural arrangements seen in malignancy; highly variable - dependent on tumour type and differentiation.
- +/-Gland formation.
- +/-Single cells.
- +/-Small clusters of cells.
Notes:
- Cytologic features of malignancy may not be present; some tumours, e.g. gallbladder carcinoma, do not always have overt cytologic features of malignancy.
- The diagnosis is based on the fact that they are foreign to the lymph node and architecturally consistent with a well-differentiated malignancy.
- Lymph node metastases in sarcomas are uncommon; they are seen in <3% of cases.[2]
- Fatty lymph nodes (esp. fatty hilus[1]) are less likely to harbor metastases.[3]
DDx - mimics of metastatic disease:
- Endometriosis.
- Ectopic decidua.[4]
- Endosalpingiosis.[5]
- Melanocytic nevus - intracapsular or within the trabeculae.[6]
- Dermatopathic lymphadenopathy.[citation needed]
- Sinus histiocytosis - especially for the junior resident.
- Tumour deposit (discoutinuous extramural extension) - definition dependent on primary tumour (e.g. in the head & neck they are tumour replaced lymph nodes, in the colon they are considered separate and not counted as lymph nodes).
Images
Mimics
See also
References
- ↑ 1.0 1.1 1.2 Mack, MG.; Rieger, J.; Baghi, M.; Bisdas, S.; Vogl, TJ. (Jun 2008). "Cervical lymph nodes.". Eur J Radiol 66 (3): 493-500. doi:10.1016/j.ejrad.2008.01.019. PMID 18337039.
- ↑ Fong, Y.; Coit, DG.; Woodruff, JM.; Brennan, MF. (Jan 1993). "Lymph node metastasis from soft tissue sarcoma in adults. Analysis of data from a prospective database of 1772 sarcoma patients.". Ann Surg 217 (1): 72-7. PMC 1242736. PMID 8424704. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1242736/.
- ↑ Korteweg, MA.; Veldhuis, WB.; Mali, WP.; Diepstraten, SC.; Luijten, PR.; van den Bosch, MA.; Eijkemans, RM.; van Diest, PJ. et al. (Feb 2012). "Investigation of lipid composition of dissected sentinel lymph nodes of breast cancer patients by 7T proton MR spectroscopy.". J Magn Reson Imaging 35 (2): 387-92. doi:10.1002/jmri.22820. PMID 21972135.
- ↑ Wu, DC.; Hirschowitz, S.; Natarajan, S. (May 2005). "Ectopic decidua of pelvic lymph nodes: a potential diagnostic pitfall.". Arch Pathol Lab Med 129 (5): e117-20. doi:10.1043/1543-2165(2005)129e117:EDOPLN2.0.CO;2. PMID 15859655.
- ↑ Corben, AD.; Nehhozina, T.; Garg, K.; Vallejo, CE.; Brogi, E. (Aug 2010). "Endosalpingiosis in axillary lymph nodes: a possible pitfall in the staging of patients with breast carcinoma.". Am J Surg Pathol 34 (8): 1211-6. doi:10.1097/PAS.0b013e3181e5e03e. PMID 20631604.
- ↑ Biddle, DA.; Evans, HL.; Kemp, BL.; El-Naggar, AK.; Harvell, JD.; White, WL.; Iskandar, SS.; Prieto, VG. (May 2003). "Intraparenchymal nevus cell aggregates in lymph nodes: a possible diagnostic pitfall with malignant melanoma and carcinoma.". Am J Surg Pathol 27 (5): 673-81. PMID 12717252.